Production of the PNA
This Pharmaceutical Needs Assessment (PNA) has been produced by Soar Beyond, contracted by Brighton & Hove City Council (BHCC).
The production has been overseen by the PNA Steering Group for Brighton & Hove Health and Wellbeing Board, with authoring support from Soar Beyond Ltd.
All data and information are accurate as of the time of writing, March 2025.
Important regulatory updates and other changes as part of the PNA process were included in August 2025 for the final document.
List of abbreviations
Abbreviations
AS – Advanced Service
AUR – Appliance Use Review
BHCC – Brighton & Hove City Council
BRM – Black and Racially Minoritised
BSA – Business Service Authority
CHD – Coronary Heart Disease
COPD – Chronic Obstructive Pulmonary Disease
CP – Community Pharmacy
CPCF – Community Pharmacy Contractual Framework
CPCS – Community Pharmacist Consultation Service
CPE – Community Pharmacy England
DAC – Dispensing Appliance Contractor
DHSC – Department of Health and Social Care
DMS – Discharge Medicines Service
DSP – Distance Selling Pharmacy
EHC – Emergency Hormonal Contraception
ES – Essential Service
EU – European Union
GP – General Practitioner
HIV – Human Immunodeficiency Virus
HLP – Healthy Living Pharmacy
HWB – Health and Wellbeing Board
ICB – Integrated Care Board
ICS – Integrated Care System
IMD – Index of Multiple Deprivation
JHWS – Joint Health and Wellbeing Strategy
JSNA – Joint Strategic Need Assessment
LAS – Local Authority-commissioned Service
LCS – Locally Commissioned Services
LES – Local Enhanced Service
LFD – Lateral Flow Device
LPC – Local Pharmaceutical Committee
LPS – Local Pharmaceutical Service
LTC – Long Term Condition
NES – National Enhanced Service
NHS – National Health Service
NHSE – NHS England
NMS – New Medicine Service
NPA – National Pharmacy Association
NRT – Nicotine Replacement Therapy
OHID – Office for Health Improvement and Disparities
ONS – Office for National Statistics
PAD – Peripheral Artery Disease
PhAS – Pharmacy Access Scheme
PNA – Pharmaceutical Needs Assessment
PCN – Primary Care Networks
PCS – Pharmacy Contraception Service
PCT – Primary Care Trust
PGD – Patient Group Direction
PLPS – Pharmaceutical Services and Local Pharmaceutical Services Regulations 2013
QOF – Quality and Outcomes Framework
RSV – Respiratory Syncytial Virus
SAC – Stoma Appliance Customisation
SCS – Smoking Cessation Service
STI – Sexually Transmitted Infection
UK – United Kingdom
Executive summary
This Pharmaceutical Needs Assessment (PNA) has been developed by Brighton & Hove Health and Wellbeing Board (HWB) in line with statutory requirements under the National Health Service (NHS) (Pharmaceutical Services and Local Pharmaceutical Services) Regulations 2013.
The purpose of the PNA is to:
- evaluate the current and future need for pharmaceutical services in Brighton & Hove
- ensure services meet the needs of the local population
- support commissioning decisions
It provides a framework for determining the adequacy of pharmaceutical provision and informs decisions about future applications to the pharmaceutical list.
Methodology
The PNA was prepared by Soar Beyond Ltd on behalf of Brighton & Hove City Council (BHCC) and overseen by a multi-stakeholder Steering Group.
A structured process was undertaken, including:
- comprehensive data gathering on pharmaceutical services and population health needs
- a public engagement exercise to understand the views on pharmacy access and use, a total of 358 responses were received
- mapping of service provision across the city and analysis of service gaps
- public and stakeholder engagement, including a 60-day consultation
- consideration of local strategies and statutory duties, including the:
- Joint Strategic Needs Assessment
- NHS Long Term Plan
- Brighton & Hove Joint Health and Wellbeing Strategy
Key findings
Brighton & Hove has a population of 279,600 (mid-year estimate 2023) with diverse demographics and a growing proportion of older adults. Health inequalities persist across the city.
There are 51 community pharmacies, including one Distance Selling Pharmacy (DSP), equating to 18.2 pharmacies per 100,000 population, slightly above the England average (18.1).
Access to pharmacies is good across the city:
- 100% of residents who have access to a car can reach a pharmacy within 10 minutes
- 98.1% of residents can walk to a pharmacy within 20 minutes
- 100% of residents can reach a pharmacy within 20 minutes using public transport
Pharmacy opening hours show:
- 35% of pharmacies open after 6 pm on weekdays
- 71% of pharmacies open on Saturdays, offering good weekend access
- 8% of pharmacies are open on Sundays, reflecting broader trends in weekend healthcare access
Advanced Services such as Pharmacy First, New Medicine Service, Flu Vaccination Service and Hypertension Case-finding are widely offered, with high uptake among providers. Enhanced Services, including COVID-19 vaccination, are also available.
Locally commissioned services (such as emergency contraception, supervised consumption, and smoking cessation) are provided across a wide pharmacy network.
No current or future gaps have been identified in the provision of Essential Services, and there is good access to other services across Brighton & Hove.
Conclusions
The 2025 PNA concludes that pharmaceutical services in Brighton & Hove are well distributed and accessible, meeting the current and projected needs of the population.
No gaps have been identified in the provision of Necessary Services during or outside normal working hours.
Advanced and Enhanced Services are widely available, and locally commissioned services contribute to improved access and public health outcomes.
The current community pharmacy network in Brighton & Hove should be supported to strengthen service delivery, particularly through:
- improved public awareness
- enhanced uptake of Advanced Services in areas of need
- alignment with local health priorities
Section 1: Introduction
1.1 Background and context
The Health Act 2009, implemented in April 2010, mandated Primary Care Trusts (PCTs) in England to undertake and publish Pharmaceutical Needs Assessments (PNAs) within specific timeframes.
The PNAs inform local commissioning decisions regarding pharmaceutical services. They provide evidence of the current and future needs for pharmaceutical services in the area, helping NHS England (NHSE), local authorities, and Integrated Care Boards (ICBs) make informed decisions about service provision and commissioning.
The PNAs are a key tool in determining market entry for new pharmaceutical services. They identify any gaps in service provision and help decide whether new pharmacies or service providers are needed to meet the pharmaceutical needs of the population.
The PNAs can contribute to public health strategies by assessing how pharmaceutical services can support broader health initiatives, such as:
- reducing hospital admissions
- promoting healthy lifestyles
- improving access to services for vulnerable populations
They help plan for future pharmaceutical service provision, ensuring the area’s needs are met as the population grows or changes, by assessing upcoming developments such as housing projects or demographic changes.
The Health and Social Care Act 2012 transferred responsibility for developing and updating PNAs to Health and Wellbeing Boards (HWBs).
PNAs are a statutory requirement, and they must be published in accordance with the NHS (Pharmaceutical Services and Local Pharmaceutical Services) Regulations 2013 (hereafter referred to as the PLPS Regulations 2013).
The PLPS Regulations, last updated in 2013 (SI 2013/349), came into force on 1 April 2013.
The initial PNAs were published in 2011 (see Table 1 for timelines).
Table 1: Timeline for PNAs
2009
Health Act 2009 introduces a statutory framework requiring Primary Care Trusts (PCTs) to prepare and publish PNAs
2011
PNAs to be published by 1 February 2011
2013
The PLPS Regulations outline PNA requirements for HWB
2015
HWB is required to publish its own PNAs by 1 April 2015
Ongoing
PNAs are reviewed every 3 years
Publication of PNAs was delayed during the COVID-19 pandemic, and PNAs were published by October 2022
This document should be revised within 3 years of its previous publication. The last PNA for Brighton & Hove HWB was published in September 2022.
This PNA for Brighton & Hove HWB fulfils this regulatory requirement.
1.2 Important changes since the last Pharmaceutical Needs Assessment (PNA)
There was an update to the PLPS Regulations in May 2023, which, in the main, was in response to the number of requests for temporary closures. Key changes were made for:
- notification procedures for changes in core opening hours
- notification procedures for 100-hour pharmacies to be able to reduce their hours to no less than 72 hours per week
- local arrangements with ICBs for the temporary reduction in hours
- all pharmacies require a business continuity plan that allows them to deal with temporary closures
Clinical Commissioning Groups (CCGs) are now replaced by Integrated Care Boards (ICBs) as part of Integrated Care Systems (ICS). In an ICS, NHS organisations, in partnership with local councils and others, take collective responsibility for:
- managing resources
- delivering NHS standards
- improving the health of the population they serve
Sussex Integrated Care Board took on the delegated responsibility for the commissioning of pharmacy services from NHS England from 1 July 2022 as an early adopter site.
Independent Prescribing ‘Pathfinder’ Programme
NHSE has developed a programme of pilot sites, referred to as ‘pathfinder’ sites, across integrated care systems, enabling an independent community pharmacist prescriber to support primary care clinical services. This presents a unique opportunity for community pharmacy to redesign current pathways and play an increasing role in delivering clinical services in primary care.
Community pharmacies
The Community Pharmacy sector has reported workforce challenges and pressures, which have been reported by the National Pharmacy Association (NPA) and Healthwatch England. Both highlighted that the current rate of pharmacy closures for 2024 was higher than in previous years, mainly due to a combination of funding and workforce challenges (source).
National analysis shows that 97% to 100% of pharmacies in England are underfunded relative to their full economic costs, raising concerns about the long-term sustainability of community pharmacy services.
Pharmacy First Service
The Pharmacy First Service commenced on 31 January 2024. It replaces the Community Pharmacist Consultation Service (CPCS). The service incorporates the elements of the CPCS, i.e. minor illness consultations with a pharmacist and the supply of urgent medicines.
In addition, consultations are available to patients under a clinical pathway for 7 clinical conditions, which have different routes of access. They can be accessed either by:
- referral from general practice
- NHS 111 and urgent and emergency care settings
- attending or contacting the pharmacy directly without referral
Hypertension Case-Finding Service
Service requirements for the Hypertension Case-Finding Service have been updated twice since the previous PNA.
The service can now be provided by suitably trained and competent pharmacy staff. Previously, only pharmacists could provide the service.
Hepatitis C testing service
This service was decommissioned from 1 April 2023.
1.3 Key upcoming changes
An announcement was made in March 2025, which included changes to some of the services and changes to the Pharmaceutical and Local Pharmaceutical Services Regulations.
Some of the key changes are listed below.
Regulation change: ability to change core opening hours. These amendments to the PLPS Regulations are intended to allow pharmacy owners greater flexibility in adjusting their opening hours to better align with the needs of patients and likely users. While the changes have not yet come into force, they are expected to take effect during the lifespan of this PNA.
DSPs will no longer be permitted to provide Advanced and Enhanced services on their premises, though remote provision will still be allowed where specified.
From 23 June 2025, no new applications for DSPs will be accepted, following amendments to the PLPS Regulations 2013, which close entry to the DSP market.
Funding and fees: Additional funding has been allocated and agreed for the Community Pharmacy Contractual Framework for 2025 to 2026.
Service developments:
- from October 2025, the Pharmacy Contraception Service will be expanded to include Emergency Hormonal Contraception (EHC)
- the New Medicine Service will be expanded to include depression from October 2025
- the Childhood Flu Vaccination Service will be trialled as an Advanced Service, which covers all children aged 2 and 3 years old from October 2025
- the Smoking Cessation Service will have Patient Group Directions (PGDs) introduced to enable the provision of Varenicline and Cytisinicline (Cytisine), no dates have been given for this
In March 2025, the government decided to merge NHS England into the Department of Health and Social Care (DHSC), aiming to reduce bureaucracy and improve the management of health services. A timeline for this is still being developed.
1.4 Purpose of the PNA
The ICB, through their delegated responsibility from NHSE, is required to publish and maintain pharmaceutical lists for each HWB area. They are required to review all application types.
Any person wishing to provide NHS pharmaceutical services is required to be included on the pharmaceutical list.
The ICB must consider any applications for entry to the pharmaceutical list, including applications to fulfil unmet needs determined within the PNA of that area or applications for benefits unforeseen within the PNA. Such applications could be for the provision of NHS pharmaceutical services from new premises or to extend the range or duration of current NHS pharmaceutical services offered from existing premises.
The PNA is the basis for the ICB to make determinations on such applications. It's therefore prudent that the PNA is compiled in line with the regulations and with due process, and that the PNA is accurately maintained and up to date.
Although decisions made by the ICB regarding applications to the pharmaceutical list may be appealed to the NHS Resolution, the final published PNA cannot be appealed.
The only challenge to a published PNA will likely be through an application for a judicial review of the process undertaken to conclude the PNA.
The PNA should be read alongside other Joint Strategic Needs Assessment (JSNA) products. The JSNA is available on the Brighton & Hove City Council website and is updated regularly. The JSNA informs Brighton & Hove’s Joint Health and Wellbeing Strategy (JHWS).
The PNA assesses how pharmaceutical services meet the public health needs identified in the JSNA, both now and in the future. By informing decisions made by the local authority and the ICB, these documents work together to improve the health and well-being of the local population and reduce inequalities.
For this PNA, at the time of writing, only services commissioned by NHSE as per the regulations have been considered as ‘NHS pharmaceutical services’.
1.5 Scope of the PNA
The PLPS Regulations 2013 detail the information required to be contained within a PNA. A PNA is required to measure the adequacy of pharmaceutical services in the HWB area under 5 key themes:
- necessary Services: current provision
- necessary Services: gaps in provision
- other relevant services: current provision
- improvements and better access: gaps in provision
- other services
In addition, the PNA details how the assessment was carried out. This includes:
- how the localities were determined
- the different needs of the different localities
- the different needs of people who share a particular characteristic
- a report on the PNA consultation
Necessary Services
The PLPS Regulations require the HWB to include a statement of those pharmaceutical services that it identifies as being necessary to meet the need for pharmaceutical services within the PNA. There is no definition of Necessary Services within the regulations, and the HWB, therefore, has complete freedom in the matter.
In Brighton & Hove, once the provision of all pharmaceutical services was identified, the HWB, via the PNA steering group, decided upon those services which were necessary to meet the pharmaceutical service for Brighton & Hove. This decision was made by service type.
Brighton & Hove HWB, through the PNA steering group, have decided that all Essential Services are Necessary Services in Brighton & Hove.
Other relevant services
These are services that the HWB is satisfied are not necessary to meet the need for pharmaceutical services, but their provision has secured improvements or better access to pharmaceutical services.
Advanced Services (excluding Smoking Cessation Service, Appliance Use Reviews, and Stoma Appliance Customisation) were agreed by the Steering Group as relevant services for the purposes of the PNA.
To appreciate the definition of ‘pharmaceutical services’ as used in this PNA, it's important to understand the types of NHS pharmaceutical providers comprised in the pharmaceutical list maintained by the ICB on behalf of NHSE. They are:
- Pharmacy contractors:
- Community Pharmacies (CPs)
- Local Pharmaceutical Service (LPS) providers
- Distance-Selling Pharmacies (DSPs)
- Dispensing Appliance Contractors (DACs)
- Dispensing doctor practices
A detailed description of each provider type and the pharmaceutical services as defined in their contract with NHSE is set out below.
1.5.1 Pharmacy contractors
Pharmacy contractors comprise both those located within the Brighton & Hove HWB areas, as listed in Appendix A, those in neighbouring HWB areas, and remote suppliers, such as DSPs.
There are 10,436 community pharmacies in England in January 2025 at the time of writing (this includes DSPs) (source).
This number has decreased from 11,071 community pharmacies since the previous PNA in 2022.
1.5.1.1 Community Pharmacies (CPs)
CPs are the most common type of pharmacy that allows the public to access their medications and advice about their health.
NHSE is responsible for administering opening hours for pharmacies, which is handled locally by ICBs through the delegated responsibility.
A pharmacy normally has 40 core contractual hours, or 72+ for those that opened under the former exemption from the control of the entry test.
These hours cannot be amended without the consent of the ICB. All applications for the amendment of hours are required to be considered and outcomes determined within 60 days, and if approved, may be implemented 30 days after approval (source).
This is due to change as mentioned in Section 1.3.
1.5.1.2 Distance-Selling Pharmacies (DSPs)
A DSP is a pharmacy contractor that works exclusively at a distance from patients. This includes mail-order and internet pharmacies that remotely manage medicine logistics and distribution.
The PLPS Regulations state that DSPs must not provide Essential Services face-to-face, but they may provide Advanced and Enhanced Services on the premises, as long as any Essential Service that forms part of the Advanced or Enhanced Service is not provided in person on the premises.
As discussed in Section 1.3, DSPs will no longer be permitted to provide Advanced and Enhanced services on their premises, though remote provision will still be allowed where specified. This is anticipated to be from October 2025.
As part of the terms of service for DSPs, provision of all services offered must be offered throughout England. It's therefore possible that patients within Brighton & Hove will receive pharmaceutical services from a DSP outside Brighton & Hove.
Figures for 2023 to 2024 show that in England, there were 409 DSPs (source), accounting for 3.4% of the total number of pharmacies. This has increased slightly from 2020 to 2021, when there were 372 DSPs, accounting for 3.2% of all pharmacy contractors.
1.5.1.3 Pharmacy Access Scheme (PhAS) providers
The PhAS has been designed to capture the pharmacies that are most important for patient access. The PhAS takes isolation and need levels into account.
Pharmacies in areas with dense provision of pharmacies remain excluded from the scheme. In areas with high numbers of pharmacies, public access to NHS pharmaceutical services is not at risk.
The scheme is focused on areas that may be at risk of reduced access, for example, where a local population relies on a single pharmacy.
DSPs, DACs, LPS contractors and dispensing General Practitioner (GP) practices are ineligible for the scheme.
From 1 January 2022, the revised PhAS is to continue to support patient access to isolated, eligible pharmacies and ensure patient access to NHS community pharmaceutical services is protected.
1.5.1.4 Local Pharmaceutical Service (LPS) providers
A pharmacy provider may be contracted to perform specified services to their local population or a specific population group.
This contract is locally commissioned by the ICB and provision for such contracts is made in the PLPS Regulations 2013 in Part 13 and Schedule 7.
Such contracts are agreed outside the national framework, although they may be over and above what is required from a national contract.
Payment for service delivery is locally agreed and funded.
1.5.2 Dispensing Appliance Contractors (DACs)
DACs operate under the Terms of Service for Appliance Contractors, as set out in Schedule 5 of the PLPS Regulations. They can supply appliances against an NHS prescription, such as stoma and incontinence aids, dressings, bandages, and more.
They are not required to have a pharmacist, do not have a regulatory body, and their premises do not have to be registered with the General Pharmaceutical Council.
DACs must provide a range of Essential Services such as:
- dispensing of appliances
- advice on appliances
- signposting
- clinical governance
- home delivery of appliances
In addition, DACs may provide the Advanced Services of Appliance Use Review (AUR) and Stoma Appliance Customisation (SAC). As of November 2024, there were a total of 111 DACs in England (source).
Pharmacy contractors, dispensing GP practices and LPS providers may supply appliances, but DACs are unable to supply medicines.
1.5.3 Dispensing GP practices
The PLPS Regulations 2013, as set out in Part 8 and Schedule 6, permit GPs in certain areas to dispense NHS prescriptions for defined populations.
These provisions are to allow patients in rural communities who do not have reasonable access to a community pharmacy to have access to dispensing services from their GP practice.
Dispensing GP practices therefore make a valuable contribution to dispensing services, although they do not offer the full range of pharmaceutical services offered at community pharmacies. Dispensing GP practices can provide such services to communities within areas known as ‘controlled localities’, which are generally rural areas with limited pharmacy access.
GP premises for dispensing must be listed within the pharmaceutical list held by NHSE, and patients retain the right of choice to have their prescription dispensed from a community pharmacy if they wish.
1.5.4 Other providers of pharmaceutical services in neighbouring areas
Two other HWBs border Brighton & Hove:
- East Sussex
- West Sussex
In determining the needs for pharmaceutical service provision to the population of Brighton & Hove, consideration has been made of the pharmaceutical service provision from the neighbouring HWB areas.
1.5.5 NHS Pharmaceutical Services
For this PNA, NHS Pharmaceutical Services are those that are contracted through the Community Pharmacy Contractual Framework (CPCF). These are commissioned nationally. The CPCF is made up of 3 types of services:
- Essential Services
- Advanced Services
- Enhanced Services
Underpinning all the services is a governance structure for the delivery of pharmacy services. This structure is set out within the PLPS Regulations 2013 and includes:
- a patient and public involvement programme
- a clinical audit programme
- a risk management programme
- a clinical effectiveness programme
- a staffing and staff programme
- an information governance programme
It provides an opportunity to audit pharmacy services and to influence the evidence base for the best practice and contribution of pharmacy services, especially to meet local health priorities within Brighton & Hove.
1.5.5.1 Essential Services (ES)
The Essential Services of the community pharmacy contract must be provided by all contractors.
ES1: Dispensing medicines
The supply of medicines and appliances ordered on NHS prescriptions, together with information and advice, to enable safe and effective use by patients and carers, and maintenance of appropriate records.
ES2: Repeat dispensing/electronic repeat dispensing (eRD)
The management and dispensing of repeatable NHS prescriptions for medicines and appliances, in partnership with the patient and the prescriber.
ES3: Disposal of unwanted medicines
Acceptance, by community pharmacies, of unwanted medicines from households and individuals which require safe disposal.
ES4: Public health (promotion of healthy lifestyles)
Each financial year (1 April to 31 March), pharmacies are required to participate in up to 6 health campaigns at the request of NHS England. This generally involves the display and distribution of leaflets provided by NHSE.
In addition, pharmacies are required to undertake prescription-linked interventions on major areas of public health concern, such as encouraging smoking cessation.
ES5: Signposting
The provision of information to people visiting the pharmacy who require further support, advice or treatment that cannot be provided by the pharmacy, or other health and social care providers or support organisations who may be able to assist them. Where appropriate, this may take the form of a referral.
ES6: Support for self-care
The provision of advice and support by pharmacy staff to enable people to derive maximum benefit from caring for themselves or their families.
ES7: Discharge Medicines Service (DMS)
From 15 February 2021, NHS trusts are able to refer patients who would benefit from extra guidance around new prescribed medicines for the provision of the DMS at their community pharmacy.
The service has been identified by NHSE’s Medicines Safety Improvement Programme to be a significant contributor to the safety of patients at transitions of care, by reducing readmissions to hospital.
ES8: Healthy Living Pharmacy (HLP)
From 1 January 2021, being an HLP is an essential requirement for all community pharmacy contractors in England.
The HLP framework is aimed at achieving consistent provision of a broad range of health promotion interventions through community pharmacies to meet local needs, improving the health and well-being of the local population and helping to reduce health inequalities.
ES9: Dispensing appliances
Pharmacists may regularly dispense appliances in the course of their business, or they may dispense such prescriptions infrequently, or they may have made a decision not to dispense them at all.
Whilst the Terms of Service requires a pharmacist to dispense any (non-Part XVIIIA listed) medicine ‘with reasonable promptness’, for appliances the obligation to dispense arises only if the pharmacist supplies such products ‘in the normal course of business’.
Brighton & Hove has designated that all Essential Services are to be regarded as Necessary Services.
1.5.5.2 Advanced Services (AS)
There are 9 Advanced Services within the Community Pharmacy Contractual Framework (CPCF).
Advanced Services are not mandatory for providers to provide, and, therefore, community pharmacies can choose to provide any of these services as long as they meet the requirements set out in the Secretary of State Directions.
The Advanced Services are listed below, and the number of pharmacy participants for each service in Brighton & Hove can be seen in Section 3.9.
AS1: Pharmacy First service
The Pharmacy First service commenced on 31 January 2024 and replaces the Community Pharmacist Consultation Service (CPCS). The service incorporates elements of the CPCS, i.e. minor illness consultations with a pharmacist and the supply of urgent medicines.
Consultations are also available to patients under a clinical pathway for 7 clinical conditions, which they can access by:
- referral from general practice
- NHS 111 and urgent and emergency care settings
- attending or contacting the pharmacy directly without referral
AS2: Flu vaccination service
A service to sustain and maximise uptake of flu vaccine in at-risk groups by providing more opportunities for access and improving convenience for eligible patients to access flu vaccinations.
AS3: Pharmacy Contraception Service (PCS)
The PCS started on 24 April 2023, allowing the ongoing supply of oral contraception from community pharmacies.
From 1 December 2023, the service included both initiation and ongoing supply of oral contraception. The supplies are authorised via a PGD, with appropriate checks, such as the measurement of the patient’s blood pressure and body mass index, being undertaken, where necessary.
As discussed in Section 1.3, from October 2025, the Pharmacy Contraception Service will be expanded to include Emergency Hormonal Contraception.
AS4: Hypertension Case-finding Service
This service was introduced in October 2021. The service has 2 stages. The first is identifying people at risk of hypertension and offering them a blood pressure measurement (a ‘clinic check’). The second stage, when clinically indicated, is offering ambulatory blood pressure monitoring.
The blood pressure and ambulatory blood pressure monitoring results will then be shared with the GP practice where the patient is registered. Patients can also be referred by the GP practice.
AS5: New Medicine Service (NMS)
The service provides support to people who are prescribed a new medicine to manage a Long-Term Condition (LTC), which will generally help them to appropriately improve their medication adherence and enhance self-management of the LTC.
Specific conditions and medicines are covered by the service. As mentioned in Section 1.3, the service will be expanded to include depression from October 2025.
AS6: Smoking Cessation Service (SCS)
This service was commissioned as an Advanced service from 10 March 2022. It enables NHS trusts to refer patients discharged from hospital to a community pharmacy of their choice to continue their smoking cessation care pathway, including providing medication and behavioural support as required, in line with the NHS Long Term Plan care model for tobacco addiction.
As mentioned in Section 1.3, the service will have PGDs introduced to enable the provision of Varenicline and Cytisinicline (Cytisine). No dates have been given for this.
AS7: Appliance Use Review (AUR)
To improve the patient’s knowledge and use of any ‘specified appliance’ by:
- establishing the way the patient uses the appliance and the patient’s experience of such use
- identifying, discussing and assisting in the resolution of poor or ineffective use of the appliance by the patient
- advising the patient on the safe and appropriate storage of the appliance
- advising the patient on the safe and proper disposal of appliances that are used or unwanted
AS8: Stoma Appliance Customisation (SAC)
This service involves the customisation of a quantity of more than one stoma appliance, based on the patient’s measurements or a template. The service aims to ensure proper use and comfortable fitting of the stoma appliance and to improve the duration of usage, thereby reducing waste.
AS9: Lateral Flow Device (LFD) service
The lateral flow device tests supply service for patients potentially eligible for COVID-19 treatments (LFD service) was commissioned as an Advanced service from 6 November 2023.
The objective of this service is to offer eligible at-risk patients access to LFD tests to enable testing at home for COVID-19, following symptoms of infection.
A positive LFD test result will be used to inform a clinical assessment to determine whether the patient is suitable for and will benefit from NICE-recommended COVID-19 treatments.
Advanced Services (excluding Smoking Cessation Service, Appliance Use Reviews, and SAC) are considered other relevant services for this PNA.
Both Essential and Advanced Services provide:
- an opportunity to identify issues with side effects or changes in dosage
- confirmation that the patient understands the role of their medicine or appliance
- opportunities for medicine optimisation
Appropriate referrals can be made to GPs or other care settings, resulting in patients receiving a better outcome from their medicines and, in some cases, cost-saving for the commissioner.
Advanced services look to support and reduce the burden on other primary care providers by allowing easier access to a healthcare professional in a high street setting.
1.5.5.3 Enhanced Services
Under the pharmacy contract, National Enhanced Services (NES) are those directly commissioned by NHSE as part of a nationally coordinated programme. There is currently one National Enhanced Service commissioned:
NES1: COVID-19 vaccination service
This service is provided by selected community pharmacies that have undergone an expression of interest process and are commissioned by NHSE. Pharmacy owners must also provide the Flu vaccination service, which is provided for a selected cohort of patients.
Local Enhanced Services (LES) are developed and designed locally by NHS England, in consultation with Local Pharmaceutical Committees (LPCs), to meet local health needs. There is one service commissioned regionally by Sussex ICB:
LES1: Bank holiday service
Provides coverage over bank holidays, Good Friday, Easter Sunday and Christmas Day, to ensure that there are pharmacies open on these days so patients can access medication if required.
Enhanced Services are considered part of the other relevant services available in Brighton & Hove for this PNA.
1.5.5.4 Other services
As stated in Section 1.4, for this PNA, ‘pharmaceutical services’ have been defined as those which are or may be commissioned under the Community Pharmacy Contractual Framework with NHSE.
Section 4 outlines services provided by NHS pharmaceutical providers in Brighton & Hove, commissioned by organisations other than NHSE or provided privately, and therefore out of scope of the PNA.
At the time of writing, the commissioning organisations primarily discussed are the local authority and Sussex ICB.
1.6 Process for developing the PNA
Brighton & Hove HWB has statutory responsibility under the Health and Social Care Act to produce and publicise a revised PNA at least every 3 years. The last PNA for Brighton & Hove was published in September 2022 and is therefore due to be reassessed and published by September 2025.
Public Health in BHCC has a duty to complete this document on behalf of the Brighton & Hove HWB. Soar Beyond Ltd was selected due to its significant experience in producing PNAs.
Step 1
Project set up and governance established between Brighton & Hove City Council Public Health, and Soar Beyond Ltd.
Step 2: Steering Group
On 23 September 2024, the Brighton & Hove PNA Steering Group was established. The terms of reference and membership of the group can be found in Appendix C.
Step 3: Project management
At this first meeting, Soar Beyond Ltd and the local authority presented and agreed on the project plan and ongoing maintenance of the project plan.
Appendix B shows an approved timeline for the project.
Step 4: Review of existing PNA and JSNA
Through the project manager, the PNA Steering Group reviewed the existing PNA and JSNA.
Step 5a: Public questionnaire on pharmacy provision
A public questionnaire to establish views about pharmacy services was agreed by the Steering Group and circulated to residents via various channels. A total of 358 responses were received.
A copy of the public questionnaire can be found in Appendix D with detailed responses.
Step 5b: Pharmacy contractor questionnaire
The Steering Group agreed on a questionnaire to be distributed to the local community pharmacies to collate information for the PNA. A total of 15 responses were received.
Due to the low response rate, the Steering Group agreed for these to not be included in the PNA.
Step 6: Mapping of services
Details of services and service providers were collated and triangulated to ensure the information that the assessment was based on was the most robust and accurate.
The Pharmacy Contracting function within the ICB, as the commissioner of service providers and services classed as necessary and relevant, was predominantly used as a base for information due to its contractual obligation to hold and maintain pharmaceutical lists on behalf of NHSE.
Information was collated, ratified and shared with the Steering Group before the assessment was commenced. The pharmaceutical list dated February 2025 was used for this assessment.
Step 7: Preparing the draft PNA for consultation
The Steering Group reviewed and revised the content and detail of the draft PNA. The process took into account the demography, health needs of residents in the local area, JSNA and other relevant strategies in order to ensure the priorities were identified correctly.
As the PNA is an assessment taken at a defined moment in time, the Steering Group agreed to monitor any changes and, if necessary, to update the PNA before finalising or publishing with accompanying supplementary statements as per the regulations, unless the changes had a significant impact on the conclusions. In the case of the latter, the group were fully aware of the need to reassess.
Step 8: Consultation
In line with the PLPS Regulations 2013, a consultation on the draft PNA was undertaken between 27 May and 27 July 2025.
The draft PNA and consultation response form was issued to all identified stakeholders. These are listed in the final PNA in Appendix E.
Step 9: Collation and analysis of consultation responses
The consultation responses were collated by the council and analysed by the Steering Group.
A summary of the responses received is noted in Appendix F, and full comments are included in Appendix G.
Step 10: Production of final PNA
The collation and analysis of consultation responses were used by the project manager to revise the draft PNA, and the final PNA was presented to the PNA Steering Group.
The final PNA was signed off by the Director of Public Health and subsequently published on the council’s website.
1.7 Localities for the PNA
The PNA Steering Group, at its first meeting, considered how the localities within Brighton & Hove geography would be defined.
The majority of health and social care data is available at the local authority city level, and this level provides reasonable statistical rigour. It was agreed that Brighton & Hove as a whole would be used as a single locality for assessment for the 2025 PNA.
Figure 1 shows the wards within Brighton & Hove and the location of the pharmacies.
A list of providers of pharmaceutical services and their locations (addresses) can be found in Appendix A.
The information contained in Appendix A has been provided by Sussex ICB, which is the ICB that covers the Brighton and Hove HWB geography. Once collated, it was ratified by the steering group during the second steering group meeting.
Figure 1: Map of Brighton & Hove HWB area showing the wards and the location of pharmacies, February 2025
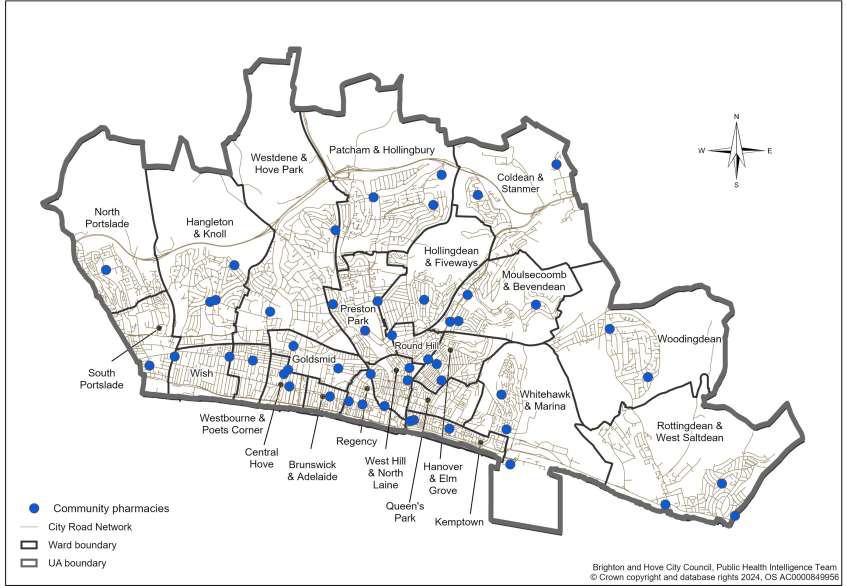
Section 2: Context for the PNA
Context for the PNA
The PNA is undertaken in the context of the health, care and wellbeing needs of the local population. These are usually laid out in the JSNA of the local area.
Based on the findings of the Joint Strategic Needs Assessment (JSNA), the Joint Health and Wellbeing Strategy (JHWS) should identify priorities and actions to improve health and well-being outcomes for the local population.
This section presents health needs data relevant to pharmacy services. It does not interpret the specific pharmaceutical service provision requirements for Brighton & Hove.
This document should be read alongside the detailed supporting documents, with relevant links provided in each subsection.
There are opportunities for the ICB and HWB to optimise Community Pharmacy Contractual Framework (CPCF) services in support of the Brighton & Hove Health and Wellbeing Strategy.
2.1 NHS Long Term Plan
The NHS Long Term Plan, published in 2019, outlines the priorities for the NHS and how it will evolve to best deliver services over a 10-year period.
These include themes such as:
- prevention and health inequalities
- care quality and outcomes
- digitally enabled care
which are approached within the context of an ageing population, funding changes and increasing inequalities.
The report places a specific focus on prevention and addressing inequalities in relation to smoking, obesity, alcohol and antimicrobial resistance and on better care for specific conditions such as:
- cancer
- cardiovascular disease
- stroke
- diabetes
- respiratory disease
- mental health
The role of community pharmacy within the NHS Long Term Plan is an important one, and one which is focused on prevention at its core.
In section 4.26 of the plan, pharmacists are described as “an integral part of an expanded multidisciplinary team”. Pharmacists “have an essential role to play in delivering the Long Term Plan”. The plan states that “…in community pharmacy, we will work with government to make greater use of community pharmacists’ skills and opportunities to engage patients…” (section 4.21).
The plan identifies that community pharmacists have a role to play in the provision of opportunities for the public to check on their health (section 3.68) and that they will be supported to identify and treat those with high-risk conditions to offer preventative care in a timely manner (section 3.69).
Pharmacists will also be expected to perform medicine reviews and to ensure patients are using medication correctly, specifically in relation to respiratory disease (3.86), which leads to the wider role that pharmacists have to play in working with general practice to help patients to take and manage their medicines, reducing wastage and reducing the likelihood of unnecessary hospital admissions (section 6.17.v).
2.2 Core20PLUS5
Core20PLUS5 is a national NHSE approach to support the reduction of health inequalities at both national and ICS levels.
The targeted population approach focuses on the most deprived 20% of the national population (CORE20) as identified by the Index of Multiple Deprivation and those within an ICS who are not identified within the core 20% but who experience lower than average outcomes, experience or access.
The ‘PLUS’ groups in Brighton & Hove are:
- carers, including young carers
- mental health transition in children and young people aged 16 to 25 years
- globally displaced communities (those seeking asylum, refugees, and vulnerable migrants)
- LGBTQ+ communities as an additional group that also experiences health inequalities and should be acknowledged through Equalities Impact Assessments (EIAs) and system-wide action
Additionally, there are 5 key clinical areas:
- maternity
- severe mental illness
- chronic respiratory disease
- early cancer diagnosis
- Hypertension Case-finding
The 10 Year Health Plan
The NHS's forthcoming 10-Year Health Plan aims to modernise healthcare in England by focusing on 3 pivotal shifts.
Transitioning care from hospitals to communities
This strategy addresses the challenges posed by an ageing population with complex health conditions and the high costs associated with hospital treatments.
By enhancing services in primary care, including community pharmacies, local health centres, and patients' homes, the plan looks to reduce hospital admissions, decrease waiting times, and promote healthier, more independent living.
Enhancing technological integration
Recognising the drawbacks of outdated systems, the plan emphasises the adoption of modern technology across the NHS. This includes:
- moving away from paper-based processes and pagers
- ensuring uniform access to advanced treatments regardless of location
- providing healthcare professionals with the tools they need to deliver efficient care
Prioritising preventive healthcare
Shifting the focus from solely treating illnesses to preventing them, the plan advocates for proactive health measures. This involves early detection initiatives, public health campaigns, and community-based programs designed to maintain wellness and reduce the incidence of serious health issues.
Collectively, these shifts aim to create a modernised NHS that delivers efficient, patient-centred care, meeting the evolving needs of the population.
The plan is due to be published in July 2025 (source).
2.4 Joint Strategic Needs Assessment (JSNA)
The purpose of JSNAs and related JHWSs (see below) is to improve health and well-being, reduce inequalities, and inform evidence-based priorities for commissioning for a specific area. They are an ongoing process of strategic assessment and planning.
The outputs guide actions for local authorities, the NHS, and partners to address health and social care needs and wider determinants of health.
The PNA should be read alongside the Brighton & Hove JSNA. Read statutory guidance about JSNAs.
The Brighton & Hove JSNA consists of a suite of reports, analysis and insights, which are constantly in a process of being refreshed and added to.
2.5 Brighton & Hove Joint Health and Wellbeing Strategy (JHWS)
Building on the evidence provided by the JSNA, the Brighton & Hove JHWS outlines the key priorities and the actions being taken to meet Brighton & Hove’s health and wellbeing needs.
The 2019 to 2030 strategy identified the following clear priorities:
- starting well: with a view to improving the health and well-being of children and young people
- living well: to improve the health and well-being of working-age adults
- ageing well: Brighton & Hove will be a place where people can age well
- dying well: To improve the experiences of those at the end of their life, whatever their age
Community pharmacy is well placed to contribute across all stages by:
- improving access to health advice on smoking, alcohol, diet, and physical activity
- supporting early detection through health checks and signposting
- delivering vaccination programmes (such as for flu and COVID-19)
- providing sexual health and contraception services
- offering mental health support and signposting to local services
- assisting carers and older adults with medicines support, falls prevention and advice
- supporting end-of-life care through palliative medication access and advice
- reaching underserved populations, including the homeless, those with substance misuse, or complex needs
Pharmacies also play a key role in reducing pressure on other providers within primary care and helping people manage long-term conditions independently within their communities.
2.6 NHS Sussex Integrated Care System Strategy
Read the NHS Sussex Integrated Care System Strategy.
In an Integrated Care System (ICS), NHS organisations, in partnership with local councils and others, take collective responsibility for managing resources, delivering NHS standards and improving the health of the population they serve.
The ICS is responsible for:
- setting the strategy and goals for improving health and care for residents in an area
- overseeing the quality and safety, decision-making, governance and financial management of services
The goal is to create a health and care system fit for the future, with transformed services that join up around the people who use them.
NHS Sussex ICB has a 5-year strategy with the vision of improving lives and reducing health inequalities across Sussex by supporting people to live healthier for longer and ensuring timely, high-quality care when needed.
The strategy reflects local priorities in Brighton & Hove while working in partnership across the wider Sussex system.
2.7 Brighton & Hove: the place
Brighton & Hove is a coastal city located in the South East of England. It's known for its diversity, creativity and seaside heritage. The city has excellent transport links and is less than one hour away from central London by train.
An understanding of the size and characteristics of the Brighton & Hove population, including how it can be expected to change over time, is fundamental to assessing population needs and planning local services.
This section provides a summary of the demographics of Brighton & Hove residents, how healthy they are, and what changes can be expected in the future.
2.7.1 Population of Brighton & Hove
This section describes the demography of people in Brighton & Hove, and includes population estimates and projections and resident profiles. The majority of the data in this chapter was sourced from various documents available from the Brighton & Hove JSNA website.
Population size, structure and composition are crucial elements in any attempt to identify, measure, and understand health and well-being.
It's important to know how many people live in an area and their demographic characteristics, such as age and gender.
2.7.1.1 Age
According to the Office for National Statistics (ONS), the latest mid-year population estimate (2023) shows that there are 279,600 estimated number of residents in Brighton & Hove. This is an increase of 5,600 people (2.1%) compared to 2012 and 1,700 (0.6%) compared to 2022.
In Brighton & Hove, in 2023, it's estimated that:
- 40,800 people (15%) are aged 0 to 15 years old
- more than two-thirds (73%, 203,700 people) are aged 16 to 66 years old
- one in ten (11%, 29,600 people) are aged 67 to 84 years old
- 5,400 people (2%) are aged 85 years or older
Brighton & Hove has a much higher proportion of people aged 19 to 31 years (23%, 64,800 people) compared to only 15% in the South East and 16% in England. The highest difference is observed between the ages of 19 to 22 years old. Nearly one in ten of Brighton & Hove's total population (9%, 26,200 people) is aged 19 to 22 years old, compared to only 4% in the South East and 5% in England.
The proportion of children aged 0 to 17 years of age is lower in Brighton & Hove (17%, 46,700 people) compared to 21% in both the South East and England.
There are also fewer people across all ages from the age of 60 years old. In Brighton & Hove, less than a fifth of the total population (19%, 54,600 people) is aged 60 years or older, compared to 26% in the South East and 25% in England.
There is both a lower proportion of children and older people in the city. This age-structure therefore gives Brighton & Hove an unusual population profile compared to the South East and England (See Figure 2 below).
Figure 2: Single year of age as a proportion of total population in Brighton & Hove, South East and England, 2023
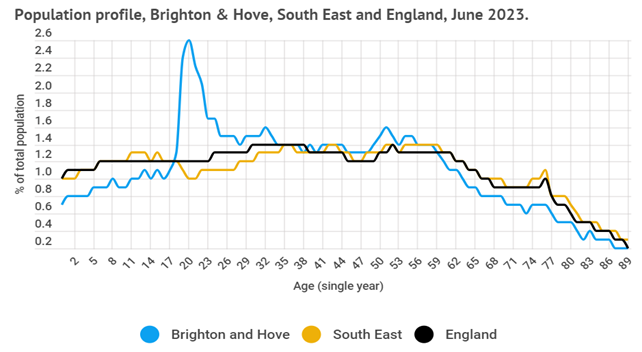
2.7.1.2 Gender
In 2023, there were estimated to be 142,800 female (51%) and 136,800 male (49%) residents in the city.
Apart from in the age range 19 to 21, there is a relatively even distribution of males and females across all ages up until the age of 75 years old.
Beyond the age of 75 years old, the proportion of female residents increases, similar to that of England. There were an estimated 18,900 residents aged 75 or older, of whom 58% (10,900 people) are female and 42% (8,000 people) are male.
By the age of 90 or older, the difference is two to one, with 1,400 female residents (67%) to 700 male residents (33%).
2.7.1.3 Ethnicity
Table 2: Ethnicity of the population in Brighton & Hove, South East and England, Census 2021 (source)
| Ethnicity | Brighton & Hove (number) | Brighton & Hove (%) | South East (%) | England (%) |
|---|---|---|---|---|
| White | 236,573 | 85.4% | 86.2% | 81.8% |
| English/Welsh/Northern Irish/British | 204,831 | 73.9% | 78.8% | 74.0% |
| Irish | 3,944 | 1.4% | 0.8% | 0.9% |
| Gypsy/Irish Traveller | 198 | 0.1% | 0.2% | 0.1% |
| Roma | 788 | 0.3% | 0.1% | 0.2% |
| White Other | 26,812 | 9.7% | 6.3% | 6.2% |
| Mixed or Multiple Ethnic Group | 13,226 | 4.8% | 2.8% | 2.9% |
| White and Black Caribbean | 2,410 | 0.9% | 0.7% | 0.9% |
| White and Black African | 2,333 | 0.8% | 0.4% | 0.4% |
| White and Asian | 4,198 | 1.5% | 0.9% | 0.8% |
| Other Mixed | 4,285 | 1.5% | 0.8% | 0.8% |
| Asian/Asian British | 13,216 | 4.8% | 7.0% | 9.2% |
| Indian | 3,636 | 1.4% | 2.6% | 3.1% |
| Pakistani | 925 | 0.3% | 1.6% | 2.7% |
| Bangladeshi | 1728 | 0.6% | 0.4% | 1.1% |
| Chinese | 3,064 | 1.1% | 0.7% | 0.7% |
| Other Asian | 3,863 | 1.4% | 1.7% | 1.6% |
| Black/African/Caribbean/Black British | 5,456 | 2.0% | 2.4% | 4.0% |
| African | 3,948 | 1.4% | 1.6% | 2.5% |
| Caribbean | 990 | 0.4% | 0.5% | 1.0% |
| Other Black | 518 | 0.2% | 0.3% | 0.5% |
| Arab | 3,051 | 1.1% | 0.3% | 0.6% |
| Any Other Ethnic Group | 5,579 | 2.0% | 1.1% | 1.6% |
| Black and Racially Minoritised | 72,270 | 26.1% | 21.0% | 25.7% |
Note: Black and Racially Minoritised is defined as all ethnic groups other than White English/Welsh/Scottish/Northern Irish/British.
Table 2 above shows that Brighton & Hove is continuing to become a more ethnically diverse city. Although the total number of residents has only increased by 1% since the last census in 2011, the number of Black and Racially Minoritised residents has increased by 35% (18,919 people) in 2021, from 19.5% (53,351) in 2011.
More than a quarter of residents (26.1%, 72,270 people) are Black and Racially Minoritised. The proportion of Black and Racially Minoritised residents in Brighton & Hove (26.1%) is significantly higher than seen in the South East (21%) but similar to what is seen in England (25.7%).
Arab residents have increased by 40% since the last census (865 people) to 3,051 residents (1.1% of the total population), higher than the South East (0.3%) and England (0.6%).
The largest Black and Racially Minoritised community in the city is White Other with 26,812 residents. This is 9.7% of the total population, making up more than a third of Black and Racially Minoritised residents (37%) and one in 10 of all residents (10%). It's also higher than the White Other population in the South East (6.3%) and England (6.2%).
The proportion of people of Mixed ethnicity in Brighton & Hove is 4.8% of the total population (13,226 people), nearly a fifth of Black and Racially Minoritised residents (18.3%). This is higher than the proportion found in the South East (2.8%) and England (2.9%). People of mixed ethnicity have increased by more than a quarter (27%, 2,818 people) since the last census.
Asian or Asian British residents have increased by 17% (1,938 people) since the last census, and now represent 4.8% of the population (13,216 people). However, the proportion is below that of the South East (7%) and nearly two times less than the proportion in England (9.2%).
The proportion of Black or Black British residents in Brighton & Hove (2%, 5,456 people) is similar to the South East (2.4%) and half that of England (4.0%). Black or Black British people have increased by nearly a third (30%, 1,268 people).
Table 3: Age profile by high-level ethnic group (source)
| Ethnic group | 0 to 24 years | 25 to 34 years | 35 to 49 years | 50 to 64 years | 65+ years |
|---|---|---|---|---|---|
| All persons (277,101) | 31% | 15% | 21% | 19% | 14% |
| White UK/British (204,831) | 29% | 14% | 20% | 21% | 17% |
| White Irish (3,944) | 17% | 13% | 23% | 28% | 19% |
| White Other (26,812) | 24% | 23% | 33% | 14% | 6% |
| Mixed/Multiple ethnic group (13,226) | 57% | 15% | 16% | 10% | 2% |
| Asian/Asian British (13,216) | 38% | 16% | 25% | 14% | 7% |
| Black/Black British (5,456) | 42% | 15% | 23% | 16% | 4% |
| Arab (3,051) | 43% | 17% | 21% | 13% | 6% |
| Any Other Ethnic group (5,579) | 31% | 17% | 26% | 17% | 9% |
| All Black and Racially Minoritised (72,270) | 35% | 19% | 26% | 14% | 6% |
2.7.1.4 Language
For nearly one in 10 Brighton & Hove residents (9%, 24,579 residents), English is not their first or preferred language. This is significantly higher than seen in the South East (7%) but similar to England (9%).
Similar to the last census, other than English, Arabic is the most widely spoken language in the city (2,620 people, 1%). This is followed by Spanish (2,507 people, 0.9%), Italian (2,221 people), Polish (1,663 people) and Portuguese (1,418 people) (source).
2.7.1.5 Population groups
Migrants (source)
The city is a destination for migrants (people living or intending to live in the city for 12 months or more) from outside the United Kingdom (UK).
The 2021 Census estimates that one in 5 residents (20%, 54,343 people) were born outside of the UK. This is similar to the 2020 ONS Country of Birth and Nationality statistics (55,000 people, 19%). The international migrant population in Brighton & Hove (20%) is significantly higher than seen in both the South East (16%) and England (17%).
More than 2 out of 5 international migrants in the city (43%, 23,104 people) were born in countries now in the European Union (EU). This is significantly higher than both the South East (38%) and England (36%). Nearly two-thirds of EU migrants in the city (65%, 15,099 people) are from EU member countries who joined the EU before 2004. This is again significantly higher than both the South East (47%) and England (44%).
Over half of the international migrants in the city (51%, 27,670 people) were from countries outside of Europe. This includes 12,517 people from the Middle East and Asia (23% of all migrants), 7,863 people from Africa and 5,326 people from the Americas and the Caribbean.
Gender identity and trans, non-binary and intersex people (source)
In the 2021 census, a total of 2,341 people aged 16 years or over (1.0%) indicated that their gender identity was different from their sex registered at birth, which equates to 1 in 100 people in Brighton & Hove. This figure is likely to be an underestimate, as some people did not respond to this question.
Gender identity estimates from Census 2021 are official statistics in development. This reflects their innovative nature and the evolving understanding of measuring gender identity, along with the uncertainty associated with these estimates. To support appropriate use, refer to the sexual orientation and gender identity quality information page before using these estimates
In Brighton & Hove, the proportion of people who indicated that their gender identity was different from their sex registered at birth was more than the proportion in England and the South East (both 0.5%).
The percentage of the population aged 16+ who identified as non-binary in the city (0.4%) is higher than the percentage in England (0.1%) and the South East (0.1%). A higher percentage of people identified as a trans man (0.2%) than in England (0.1%) and the South East (0.1%). The percentage who identified as a trans woman was similar to England and the South East (all 0.1%).
Brighton & Hove has the 21st highest percentage of people whose gender identity was different from their sex registered at birth, out of 309 local authorities in England.
In addition, as Brighton & Hove is seen as inclusive, many trans people who live elsewhere visit Brighton & Hove to socialise, study, and/or work.
Data suggest that trans and non-binary people in Brighton & Hove:
- have a younger population distribution than the overall population, although trans people are represented in all age groups
- have diverse gender identities
- are more likely to have limiting long-term health or disability than the overall population
- are dispersed across ethnic groups
- live across all areas of Brighton & Hove, ranging from 0.3% in West Blatchington to 1.7% in Hanover, and with many of Hanover’s surrounding Middle-layer Super Output Areas above 1.5% and above 1% in many central and university corridor areas of the city
Lesbian, gay and bisexual
According to the 2021 UK Census, a total of 25,250 people aged 16 and over (11%) said that their sexual orientation was Lesbian, Gay, Bisexual (LGB+) (“Gay or Lesbian”, “Bisexual” or “Other sexual orientation”), about 3.5 times higher than the South East (3%) and England (3%) (source).
People with long-term health problems or disability
According to the 2021 census, 20,351 people (7%) of the resident population in Brighton & Hove have their day-to-day activity ‘limited a lot’ due to a long-term health problem or disability.
A further 31,466 people (11%) have their day-to-day activity ‘limited a little’. This is similar to the proportions found in the South East and England.
Neurodiversity - autism
The number of autistic children in Brighton & Hove has been increasing since 2015.
In 2015, there were 301 autistic children known to schools (8.1 per 1,000 population), lower than England (10.8 per 1,000 population). However, in 2020, the numbers rose to 766 (23.9 per 1,000 population), higher than England (18.0 per 1,000 population). This is an increase of 465 autistic children since 2015.
The current figure is also likely to be an underestimate (source).
Provision of unpaid care
According to the 2021 census, 20,804 people in the city (8%) provide some amount of unpaid care each week to either a family member, friend or neighbour who has either a long-term illness or disability or problems related to age. This is a 13% decrease since 2011 (3,163 fewer people).
4% of the total population (11,334) of those providing unpaid care do so for one to 19 hours a week, similar to the South East (4%) and England (4%). 2% of the total population (5,430) provide unpaid care of 50 hours or more a week.
The proportion of residents providing unpaid care (8%) is similar to England (8% overall) and the South East (9%) (source).
Armed forces personnel
At the time of the 2021 census, around 1 in 40 people (2%, 5,618 people) aged 16 years or over in Brighton & Hove had previously served in the UK Armed Forces. This is lower than the South East (4.2%) and England (3.8%). Of these, 70% (3,949 people) served in the regular armed forces, 25% (1,423 people) in the reserves and 246 (4%) in both.
4% of the households in the city (5,292 households) have at least one person who has previously served (source).
Students
For the academic year 2021 to 2022, there were 37,700 students at the University of Sussex and the University of Brighton. This was an increase of 1.3% (500 students) compared to 2020 to 2021. In England, there has been a 3.9% increase in the number of students over the same period.
In Brighton & Hove in 2021 to 2022, 58% of students were female (22,030 people) compared to 42% male (15,455 people).
It should be noted that not all students at the 2 universities live in Brighton & Hove.
Visitors
The city is a popular tourist destination. In 2022, around 10.0 million trips were estimated to have been made to the city by day visitors (down 6.5% on 2019), with over 5.2 million overnight stays (down 4.8% on 2019) (source).
People experiencing homelessness
An estimated 1,617 households were living in temporary accommodation arranged by the council in June 2024 (source).
During the Street Count by the Rough Sleeper Team in 2023, 52 street homeless people were identified (source).
Offenders
There were 1,764 offenders resident in Brighton & Hove from January to December 2022 (source).
2.7.2 Population projections - 2023 to 2033
The Office for National Statistics has delayed publication of population projections, rebased for Census 2021 to 2025. Given the changes in the population estimates for the city in the 2021 Census, we cannot use the previous ONS published population projections.
The table below shows the modelled estimates for the projected change in population by broad age group between 2023 and 2033 for Brighton & Hove.
Table 4: Brighton & Hove modelled estimates for projected change in population by broad age group between 2023 and 2033 (source)
| Age group | 2023 | 2033 | Change (number) | Change (%) |
|---|---|---|---|---|
| Under 16 | 40,767 | 33,069 | -7,697 | -18.9% |
| 16 to 64 | 197,743 | 202,322 | 4,579 | 2.3% |
| 65+ | 40,070 | 49,905 | 9,835 | 24.5% |
| Total | 278,580 | 285,297 | 6,717 | 2.4% |
The council modelled estimates for the housing planning to 2033 project an increase of around 6,700 people (2% increase). The population aged 65+ is projected to see a larger increase, rising by 9,800 people (25%).
There are approximately 84 care homes in the city.
A further reduction in the number of children and young people is projected (19% reduction).
2.7.3 Household projections
2.7.3.1 Households
According to the 2021 census, there are 121,400 households with at least one resident in Brighton & Hove, a decrease of 139 households (0.1%) compared to the 2011 Census (source).
More than a third of households (35%, 42,101 homes) in the city are single-person households, higher than seen in the South East (28%) and England (30%).
Nearly a quarter of households (24%, 28,687 homes) contain a dependent child aged under 16, lower than the South East (29%) and England (28%). Compared to the 2011 census, the number of households with dependent children has reduced by 4%.
The city has a similar proportion of lone parent households (6%, 7,229 homes) as the South East (6%) and England (7%). Compared to the 2011 Census, the number of lone-parent families has fallen by 16% (1,408 homes).
A third of single-person households (13,875 homes) and one in 10 of all households (11%) are households with a single person aged 66 or older living there, which is also higher than seen in the South East (13%) and England (13%).
2.7.3.2 Housing and regeneration plans
The Strategic Housing Land Availability Assessment (SHLAA) Update 2023 describes the housing supply position for Brighton & Hove. There are 1,716 new units of housing planned during the lifetime of this PNA between 2025 to 2026, and 2027 to 2028.
There will be a supply of 864 (6+) units built in development areas in the city between 2025 to 2026, and 2027 to 2028.
Table 5 shows that the Hove Station and Lewes Road areas will see the largest amount of new housing supply.
Table 5: Identified supply of 6+ units in development areas between 2025/26 and 2027/28
| Development area | 2025 to 2026 | 2026 to 2027 | 2027 to 2028 | Total |
|---|---|---|---|---|
| Brighton Marina & Black Rock | 0 | 0 | 100 | 100 |
| Hove Station | 174 | 64 | 0 | 238 |
| Brighton Station/London Road | 116 | 0 | 0 | 116 |
| Lewes Road | 158 | 100 | 0 | 258 |
| Shoreham Harbour | 0 | 0 | 52 | 52 |
| Toads Hole Valley | 0 | 0 | 100 | 100 |
| Total | 448 | 164 | 252 | 864 |
2.7.4 Deprivation
Out of 317 local authorities, Brighton & Hove is ranked the 131st most deprived authority in England according to the 2019 Index of Multiple Deprivation (IMD).
In 2019, 17% of the population of the city lived in one of the 20% most deprived areas in England, and 13% lived in one of the 20% least deprived areas in England.
Some areas are more affected by deprivation than others. The highest concentration of deprivation is in Whitehawk, Moulsecoomb, and Hollingbury. Along the coast, to the west of the city and in Woodingdean, there are also pockets of deprivation. All these areas are in the 20% most deprived areas in England (source).
2.8 Health of the population
All data used are from Fingertips (accessed during November 2024), unless stated otherwise. See Fingertips for indicator definitions and notes on data quality.
2.8.1 Life expectancy
Between 2021 and 2023, the average life expectancy in the city was 78.8 years for males and 83.2 years for females. Both genders have similar life expectancy to England (England: males 79.1 years, females 83.1 years).
Between 2021 and 2023, the average healthy life expectancy was 60.6 years for males and 61.5 years for females. Both genders have similar healthy life expectancy to England (England: males 61.5 years, females 61.9 years).
The average number of years for those living in the most deprived area of the city is 9.1 years less for males and 7.7 years less for females, compared to those living in the least deprived areas (2018 to 2020). Average healthy life expectancy is 14.0 years less for males and 12.5 years for females (2009 to 2013).
2.8.2 Health behaviours
2.8.2.1 Teenage conceptions
The rate of under-18s conceptions in Brighton & Hove in 2021 was 9.9 per 1,000 population. This is similar to the England average of 13.1 per 1,000 population, and there has been a recent decrease in the trend.
2.8.2.2 Sexually Transmitted Infections (STIs)
In 2023, Brighton & Hove had a higher new STI diagnosis rate (1,249 per 100,000 population) than the South-East region (369 per 100,000) and England (520 per 100,000).
In past years, although the new Human Immunodeficiency Virus (HIV) diagnosis in the city had been decreasing, the rates were still worse than in England. However, since 2022, the new HIV diagnosis rate for the city was similar to the England average, and in 2023 the rate was 11.1 per 100,000 population, not significantly different to South East (9.9 per 100,000 population) and similar to England (10.4 per 100,000 population).
2.8.3 Health profiles
Health profiles have been produced for each local authority by the Office for Health Improvement and Disparities (OHID). The profile consists of over 30 indicators grouped under the following 7 main domains:
- life expectancy and causes of death
- injuries and ill health
- behavioural risk factors
- health protection
- child health
- inequalities
- wider determinants of health
The purpose of the profile is to help the local government and commissioning health services make strategic plans to improve the health of their local population and reduce health inequalities.
Performance for local authorities in England is benchmarked against the England average for specified indicators in Brighton & Hove.
Figure 3: Health indicators for Brighton & Hove compared to England (source)
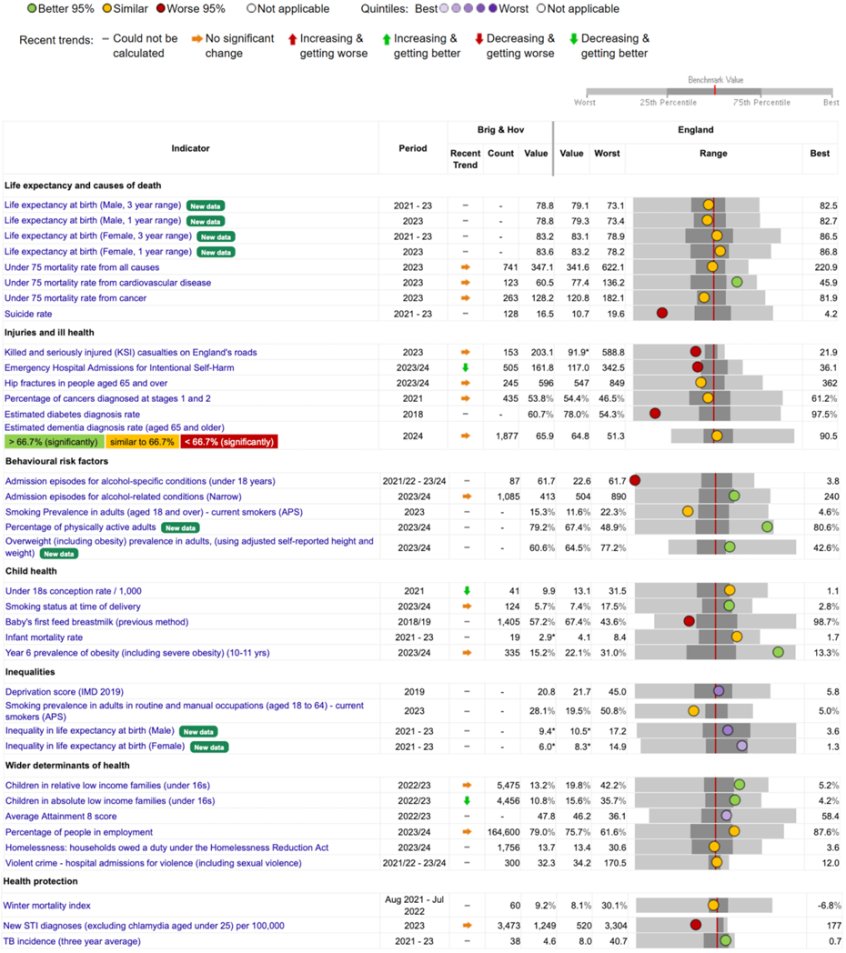

Figure 3 shows that, for the following indicators, performance in Brighton & Hove is significantly worse than the England average (source):
- life expectancy and causes of death: suicide rate (persons, 10+ years) (2021 to 2023)
- injuries and ill health:
- killed and seriously injured on the road (2022)
- emergency hospital admissions with intentional self-harm (2022 to 2023)
- estimated diabetes diagnosis rate (2018)
- behavioural factors: under-18 admission episodes for alcohol-specific conditions (2020 to 2021, and 2022 to 2023)
- child health: baby’s first feed breastmilk, previous method (2018 to 2019)
- health protection: new STI diagnoses (excluding chlamydia aged under 25) per 100,000 (2023)
2.8.3.1 Suicide rate (persons, 10+ years) (2021 to 2023)
The suicide rate for persons 10 years and above in 2021 to 2023 was 16.5 per 100,000 population in Brighton & Hove, 10.4 per 100,00 population in South-East, and 10.7 per 100,000 population in England.
2.8.3.2 Killed and seriously injured casualties on England’s roads (2022)
In 2023, the number of people reportedly killed, all ages, was 203.1 per billion vehicle miles travelled in Brighton & Hove. The numbers for South-East and England are estimated to be 89.8 per billion vehicle miles and 91.9 per billion vehicle miles, respectively.
2.8.3.3 Emergency hospital admissions for intentional self-harm (2022 to 2023)
In 2022 to 2023, the rate of emergency hospital admission in Brighton & Hove was 174.4 per 100,000 population, 138.3 per 100,000 population in the South-East region, and 126.3 per 100,000 population in England.
2.8.3.4 Estimated diabetes diagnosis rate (2018)
In 2018, the estimated diabetes diagnosis rate in Brighton & Hove was 60.7%, lower than the South-East 75.2% and England 78.0%.
2.8.3.5 Under 18 admission episodes for alcohol-specific conditions (2020 to 2021 and 2022 to 2023)
Within this period, there were 80 under-18s (56.4 per 100,000 population) admitted for alcohol-specific conditions in Brighton & Hove, 28.6 per 100,000 in the South-East, and 26.0 per 100,000 in England.
2.8.3.6 Baby’s first feed breastmilk previous method (2018 to 2019)
In 2018 to 2019, the proportion of babies whose first feed was breastmilk in Brighton & Hove was 57.2%, significantly lower than South-East (72.7%) and England (67.4%).
2.8.3.7 New STI diagnoses (excluding chlamydia aged under 25) per 100,000 (2023)
In 2023, Brighton & Hove had a significantly higher rate of new STI diagnoses (1,249 per 100,000) than South-East (369 per 100,000) and England (520 per 100,000).
2.8.4 Mental health
In 2022 to 2023, the recorded prevalence of depression among adults (18+) on GP records was 13.4% for Brighton & Hove. This is similar to the South East (13.8%) and England (13.2%).
Comparing these rates with previous years, there seems to be an increasing trend in depression in Brighton & Hove, the South-East region, and England.
The percentage of adults on GP Severe Mental Illness Registers in 2020 to 2021 was 1.29% in Brighton & Hove, 0.86% in the South East Region and 0.95% in England.
2.9 Burden of disease
Table 6 and Figure 4 show the Quality and Outcomes Framework (QOF) prevalence for Long Term Conditions (LTCs) in Brighton & Hove.
QOF data shows recorded prevalence; therefore, the anticipated prevalence may be higher with unmet need for the conditions which contribute to premature mortality.
Table 6: Percentage of patients recorded on GP practice disease registers for long-term conditions
| Condition | Area | Count | Value | 99.8% Lower CI | 99.8% Upper CI |
|---|---|---|---|---|---|
| Cancer | England | 2,300,426 | 3.6% | 3.6% | 3.6% |
| Cancer | Brighton & Hove | 9,553 | 2.9% | 2.8% | 3% |
| Heart failure | England | 672,409 | 1.1% | 1.1% | 1.1% |
| Heart failure | Brighton & Hove | 2,261 | 0.7% | 0.6% | 0.7% |
| Asthma | England | 3,886,879 | 6.5% | 6.5% | 6.5% |
| Asthma | Brighton & Hove | 19,374 | 6.1% | 5.9% | 6.2% |
| Atrial fibrillation | England | 1,375,120 | 2.2% | 2.2% | 2.2% |
| Atrial fibrillation | Brighton & Hove | 5,478 | 1.6% | 1.6% | 1.7% |
| Stroke | England | 1,175,341 | 1.9% | 1.9% | 1.9% |
| Stroke | Brighton & Hove | 4,552 | 1.4% | 1.3% | 1.4% |
| Diabetes | England | 3,938,080 | 7.7% | 7.6% | 7.7% |
| Diabetes | Brighton & Hove | 13,479 | 4.7% | 4.6% | 4.8% |
| Coronary Heart Disease (CHD) | England | 1,879,149 | 3% | 3% | 3% |
| CHD | Brighton & Hove | 6,968 | 2.1% | 2% | 2.2% |
| Peripheral Artery Disease (PAD) | England | 353,814 | 0.6% | 0.6% | 0.6% |
| PAD | Brighton & Hove | 1,346 | 0.4% | 0.4% | 0.4% |
| Hypertension | England | 9,350,858 | 14.8% | 14.8% | 14.8% |
| Hypertension | Brighton & Hove | 33,913 | 10.2% | 105% | 10.3% |
| Chronic Obstructive Pulmonary Disease (COPD) | England | 1,175,163 | 1.9% | 1.9% | 1.9% |
| COPD | Brighton & Hove | 5,178 | 1.6% | 1.5% | 1.6% |
| Rheumatoid Arthritis | England | 403,782 | 0.8% | 0.8% | 0.8% |
| Rheumatoid Arthritis | Brighton & Hove | 1,525 | 0.5% | 0.5% | 0.6% |
Figure 4: Recent trends of QOF prevalence in Brighton & Hove and comparison with England
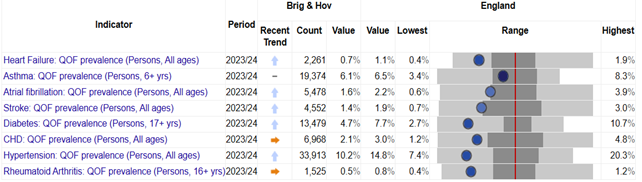
Burden of disease summary
The prevalence of long-term conditions recorded in GP practices in Brighton & Hove is generally lower than the national average across most conditions. This may be linked to the prevalence of its younger population (Table 6 and Figure 4).
Section 3: NHS pharmaceutical services provision, currently commissioned
3.1 Overview
There is a total of 51 contractors in Brighton & Hove.
Table 7: Contractor type and number in Brighton & Hove
| Type of contractor | Number |
|---|---|
| 40-hour community pharmacies (including five PhAS providers) | 50 |
| 72-hour plus community pharmacies | 0 |
| Distance Selling Pharmacies | 1 |
| Local Pharmaceutical Service providers | 0 |
| Dispensing Appliance Contractors | 0 |
| Dispensing GP Practices | 0 |
| Total | 51 |
A list of all contractors in Brighton & Hove and their opening hours can be found in Appendix A.
Figure 5 shows all contractor locations within Brighton & Hove and surrounding areas, showing that there are 4 pharmacies to the west of the city within a 1-mile radius. These are all within the West Sussex County Council.
Figure 5: Map of pharmacies in Brighton & Hove and neighbouring areas in a 1.6km/ 1 mile buffer
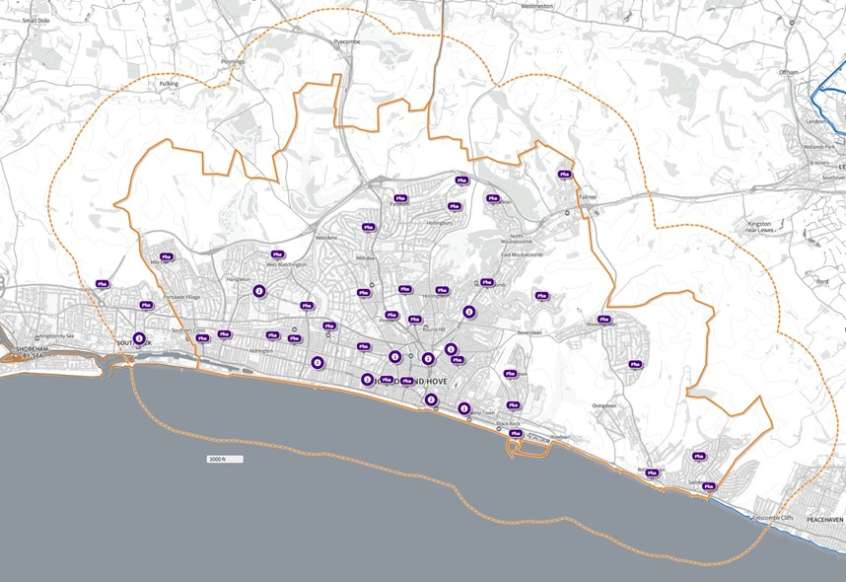
3.2 Community pharmacies (including Distance Selling)
Table 8: Number of community pharmacies in Brighton & Hove
| Number of community pharmacies | Population of Brighton & Hove | Ratio of pharmacies per 100,000 population |
|---|---|---|
| 51 (includes one DSP) | 279,600 | 18.2 |
Correct as of 26 February 2025.
Community pharmacies are described in Section 1.5.1.1. There are 51 community pharmacies in Brighton & Hove, which has decreased from 53 in the last PNA.
The average number of community pharmacies per 100,000 across Brighton & Hove is 18.2, which is similar to the England average of 18.1 community pharmacies per 100,000 population.
A number of community pharmacies have been closing across the country due to funding and workforce pressures over the last 10 years.
There is no benchmark or specific guidance on how many community pharmacies per 100,000 there should be, and this is only an indication of capacity per pharmacy.
Distance Selling Pharmacies are described in Section 1.5.1.2. There is one DSP in Brighton & Hove; however, residents are able to access other DSPs across England, as services are provided nationally by DSPs.
Table 9: Average number of community pharmacies in 100,000 population
| Area | Number of community pharmacies | Total population | Average no. of community pharmacies per 100,000 population |
|---|---|---|---|
| Brighton & Hove | 51 | 279,600 | 18.2 |
| England | 10,436 | 57,690,323 | 18.1 |
Section 1.5.5.1 lists the Essential Services of the pharmacy contract. It's assumed, due to the contractual obligation, that provision of all these services is available from all contractors.
Analysis of dispensing data has highlighted approximately 399,323 prescription items dispensed each month (between August and October 2024), accounting for a monthly average of 7,830 items per community pharmacy in Brighton & Hove (source). This is higher than the England average of 7,109 and the South East average of 6,953 items per pharmacy monthly in 2024 to 2025 (source).
Further analysis of the pharmaceutical service provision and health needs is explored in Section 6.
3.3 Local Pharmaceutical Service (LPS) providers
LPS providers are described in Section 1.5.1.4.
There are no LPS pharmacies in Brighton & Hove.
3.4 Dispensing Appliance Contractors (DACs)
DACs are described in Section 1.5.2.
There are no DACs in Brighton & Hove.
3.5 Dispensing GP practices
Dispensing GP Practices are described in Section 1.5.3.
There are no dispensing GP practices in Brighton & Hove.
As part of the Essential Services of appliance contractors, a free delivery service is available to all patients. It's therefore likely that patients will obtain appliances delivered from DACs outside Brighton & Hove. There are 112 DACs in England (source).
3.6 Pharmacy Access Scheme (PhAS) pharmacies
The Pharmacy Access Scheme is described in Section 1.5.1.3.
There are 5 PhAS providers in Brighton & Hove, and details of these can be found in Appendix A.
3.7 Pharmaceutical service provision provided from outside Brighton & Hove
Brighton & Hove borders 2 other HWBs, East Sussex and West Sussex, and has good transport links. Population in certain areas of Brighton & Hove may therefore find community pharmacies in neighbouring HWB areas more accessible and/or more convenient.
It's not practical to list here all those pharmacies in other areas by which Brighton & Hove residents will access pharmaceutical services, but there are 4 community pharmacies within a one-mile (1.6 kilometre) buffer zone from the local authority boundary.
There is one significant pharmacy that the Steering Group would like to mention, in West Sussex, 1.5 miles to the west of the city’s boundary:
• Tesco Pharmacy located in the Holmbush Shopping Centre (BN43 6TJ)
3.8 Access to community pharmacies
Community pharmacies in Brighton & Hove are particularly located around areas with a higher density of population and higher levels of deprivation (from IMD 2019), as seen in Figures 6 and 7 below.
Figure 6: Map of pharmacies in Brighton & Hove with population density
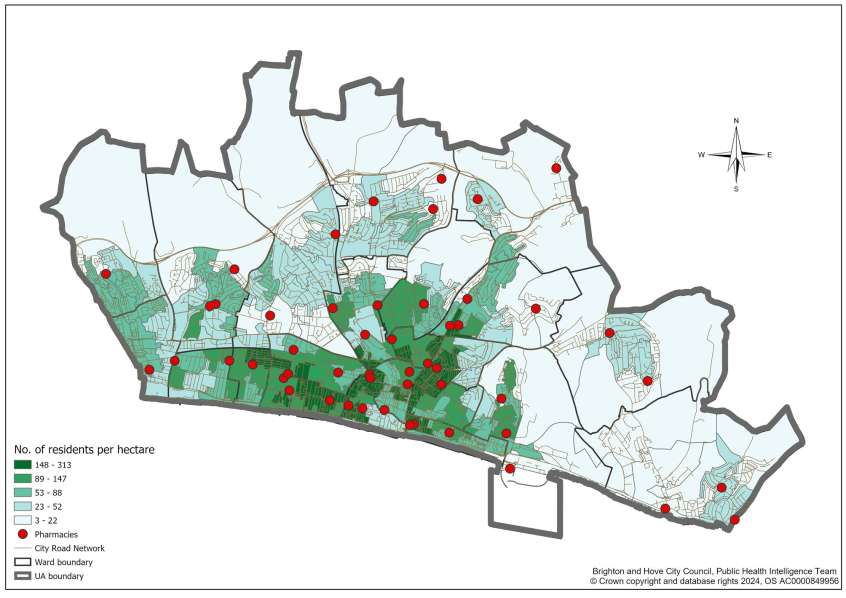
Figure 7: Map of pharmacies in Brighton & Hove with the Index of Multiple Deprivation
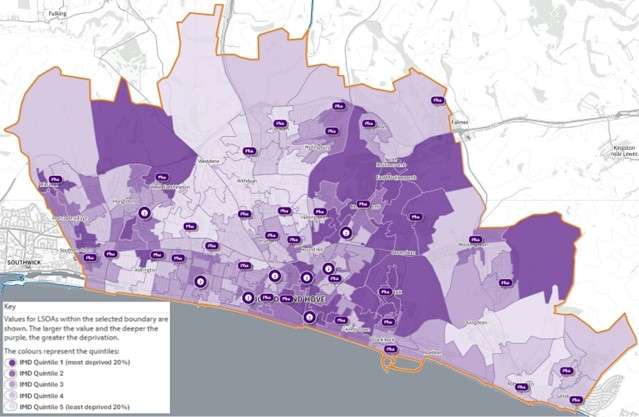
A previously published article suggests:
- 89% of the population in England has access to a community pharmacy within a 20-minute walk, but this falls to 14% in rural areas
- over 99% of those in areas of highest deprivation are within a 20-minute walk of a community pharmacy
The same study found that access is greater in areas of high deprivation. Higher levels of deprivation are linked with increased premature mortality rates and, therefore, greater health needs.
While this is based on a relatively old publication, it still remains a useful reference in the absence of more recent data.
A list of community pharmacies and their opening hours can be found in Appendix A.
3.8.1 Travelling to a community pharmacy
3.8.1.1 Car or van availability
Census 2021 data shows that the overall percentage of households that have access to a car or van is 62.6% in Brighton & Hove, compared to 83.1% in the South East and 76.5% in England (source).
However, car ownership varies across the city. Between 50% and 78% of households in the centre of Brighton & Hove have no access to a car or van compared to 6% to 15% in some areas outside of the city centre (see Figure 8).
Table 10: Percentage of households across Brighton & Hove with access to at least one car or van
| Area | Households with access to a car or van |
|---|---|
| Brighton & Hove | 62.6% |
| South East | 83.1% |
| England | 76.5% |
Figure 8. Map of the distribution of households without access to a car or van
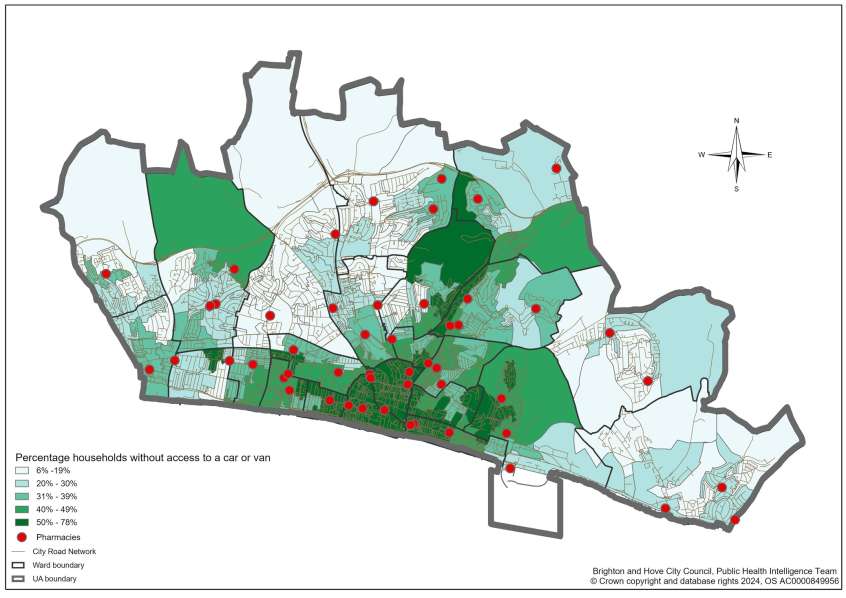
3.8.1.2 Time taken to get to a community pharmacy
The following maps and table below show travel times to community pharmacies using a variety of options.
The methodology applied through the nationally approved SHAPE tool is as follows:
Walk: by time: assumes walking speed of 5km/hour (3.1 miles/hour).
Walk: by distance: uses lengths of paths and roads with pedestrian access.
Car: by distance: uses the length of all roads.
Car: by time: calculated using the normal speed limits, but takes into account junctions, crossings and traffic lights, the rush hour option uses additional congestion data and road density analysis. Validated with similar data on Google Maps.
Public transport: experimental: uses buses, trams and rail, but coverage across some areas may be inconsistent. Options allow travel either to or from the sites and selection of weekday morning, afternoon and evening travel times.
The algorithm for calculating the distances that can be travelled from any point assumes that someone can walk from the start location, catch a bus or a train from a known stop, get off at another stop and potentially walk again, or even catch another bus or train.
Generally, it works best when used for a single selected site, rather than multiple sites.
Table 11: Time to pharmacy with various methods of transportation across Brighton & Hove
| Transport method | Time | Population within time band |
|---|---|---|
| Car (weekday morning) | 10 minutes | 278,370 (100%) |
| Walk | 20 minutes | 272,947 (98.1%) |
| Public transport (weekday morning) | 20 minutes | 278,370 (100%) |
Source: SHAPE Tool.
There are also a number of accessible disabled bays to park in to improve access for those who have a disability.
Figure 9: Map to show all the parking bays marked as disabled in relation to the community pharmacies across Brighton & Hove
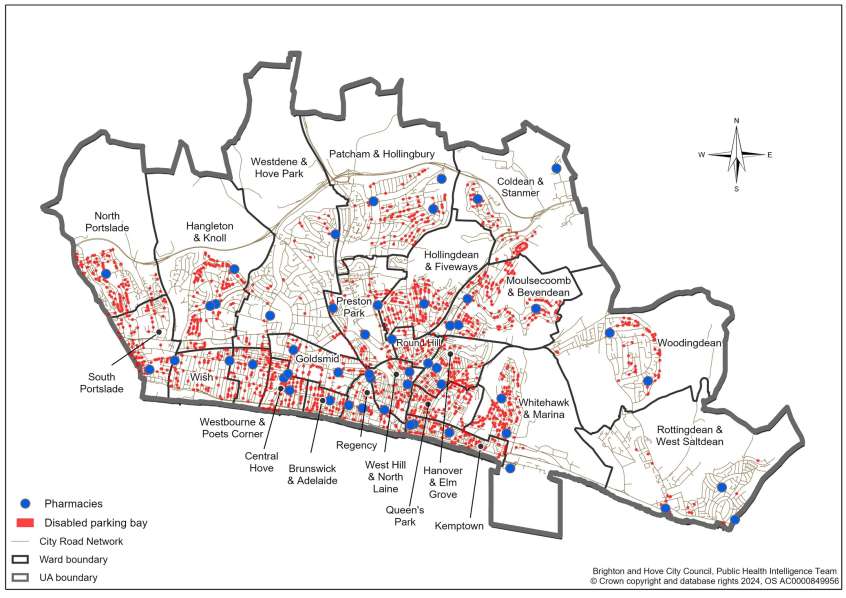
In summary:
- 100% of the population who have access to a vehicle in Brighton & Hove can get to a pharmacy within 10 minutes by private transport (Figure 11)
- 98.1% of the population who can walk can get to the nearest pharmacy within 20 minutes (Figure 10)
- 100% have access to a pharmacy within a 20-minute journey by public transport (Figure 12)
The areas not within a 20-minute walk are:
- some streets and neighbourhoods between Portslade and Hangleton
- streets in North Hangleton, south of the A27 bypass
- parts of Westdene
- a few properties at the top of Braypool Lane and the surrounding properties around Waterhall Road
- a few streets north of Easthill Park, in the east of Portslade Village
- a few streets around and between Bevendean and Woodingdean
- part of East Moulsecoomb and North Moulsecoomb, including some student accommodation at Brighton University, Falmer
- Stanmer Village
- parts of Ovingdean
- Roedean
- a few streets in north Saltdean
Figure 10: Map of average walk times to community pharmacies in Brighton & Hove
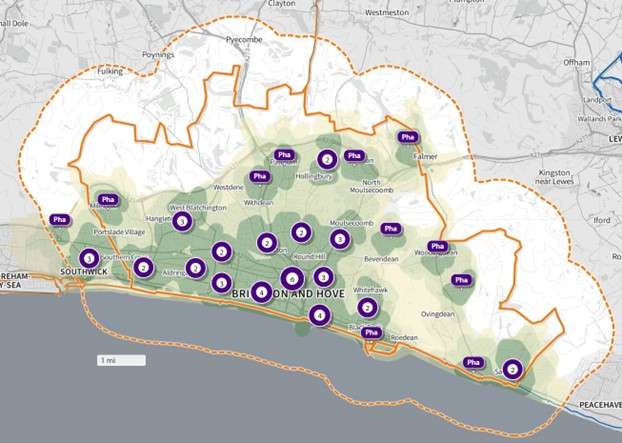
Figure 11: Map of drive times by private transport to the nearest pharmacy in Brighton & Hove (weekday morning)
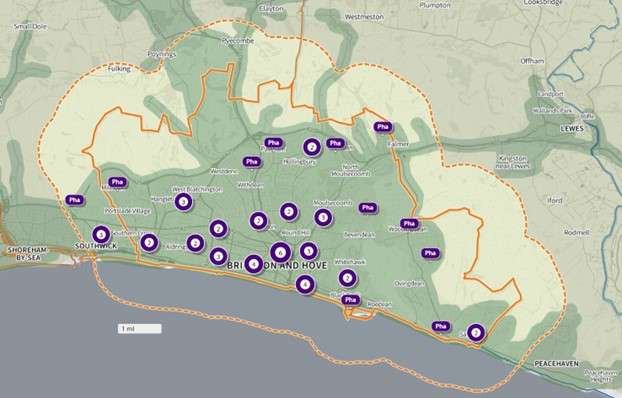
Figure 12: Map of public transport times to the nearest pharmacy in Brighton & Hove (weekday morning)
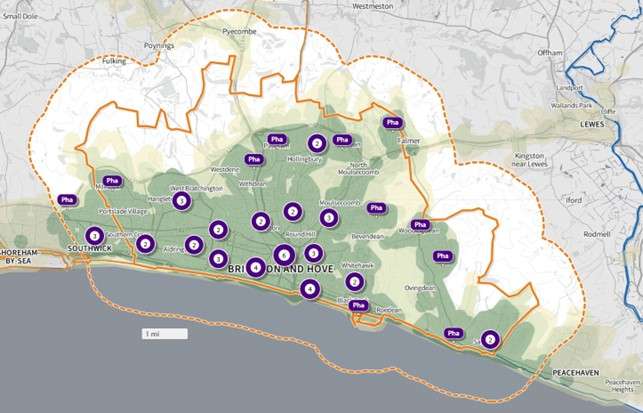
3.8.2 Weekend and evening provision
In May 2023, the PLPS Regulations were updated to allow 100-hour pharmacies to reduce their total weekly core opening hours to no less than 72 hours, subject to various requirements.
In the 2022 PNA, Brighton & Hove had no 100-hour pharmacies, and due to there being no mechanism for market entry for a new one, the number has remained the same.
Nationally, there has been a decline in the number of 100-hour community pharmacies in England open in 2022, which was 9.4%, and now for 72 hours or more per week is 7.7%.
Despite not being any pharmacy open for 72 hours or more, there are a number of community pharmacies open in the evenings and weekends.
Table 12: Number and percentage of community pharmacy providers (including DSPs) open Monday to Friday (excluding bank holidays) beyond 6 pm, and on Saturday and Sunday
| Area | Number (%) of pharmacies open beyond 6 pm | Number (%) of pharmacies open on Saturday | Number (%) of pharmacies open on a Sunday |
|---|---|---|---|
| Brighton & Hove | 18 (35%) | 36 (71%) | 4 (8%) |
3.8.3 Routine weekday evening access to community pharmacies
There are 18 (35%) community pharmacy providers open beyond 6 pm, Monday to Friday (excluding bank holidays) in Brighton & Hove, as shown in Figure 13 below, and pharmacies’ opening hours are listed in Appendix A.
Figure 13: Map of pharmacy opening hours in Brighton & Hove (weekday evening)
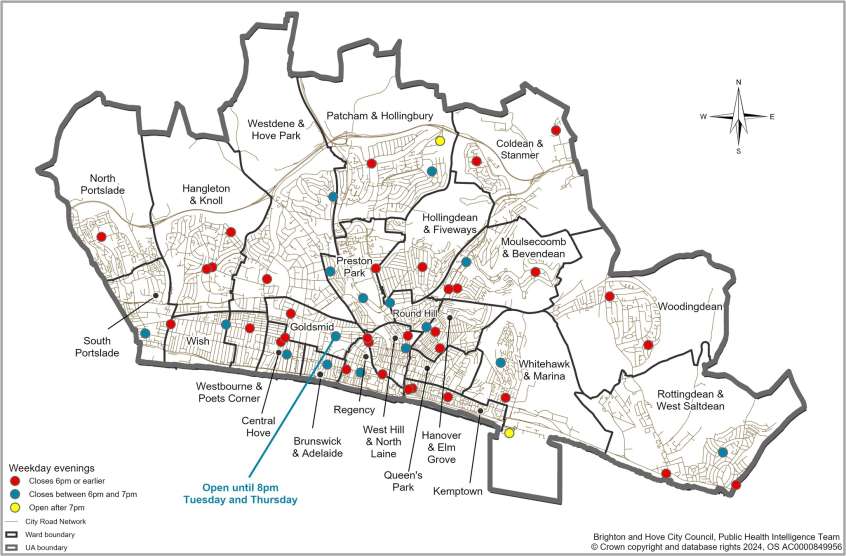
3.8.4 Routine Saturday daytime access to community pharmacies
There are 36 (71%) community pharmacy providers open on Saturdays in Brighton & Hove. These can be seen in Figure 14 below, and the full details of all pharmacies’ opening hours are listed in Appendix A.
Pharmacies open on Saturday evening are primarily located along the central spine of the city, reflecting areas of higher footfall and population density.
In peripheral areas such as Patcham & Hollingbury, Woodingdean, and Rottingdean & West Saltdean, Saturday pharmacy access is more limited, with some pharmacies only open in the morning or closed.
Overall, Saturday access across the city is good, particularly in areas of highest demand, helping to ensure residents can access pharmacy services over the weekend.
Figure 14: Map of pharmacy opening hours in Brighton & Hove (Saturday)
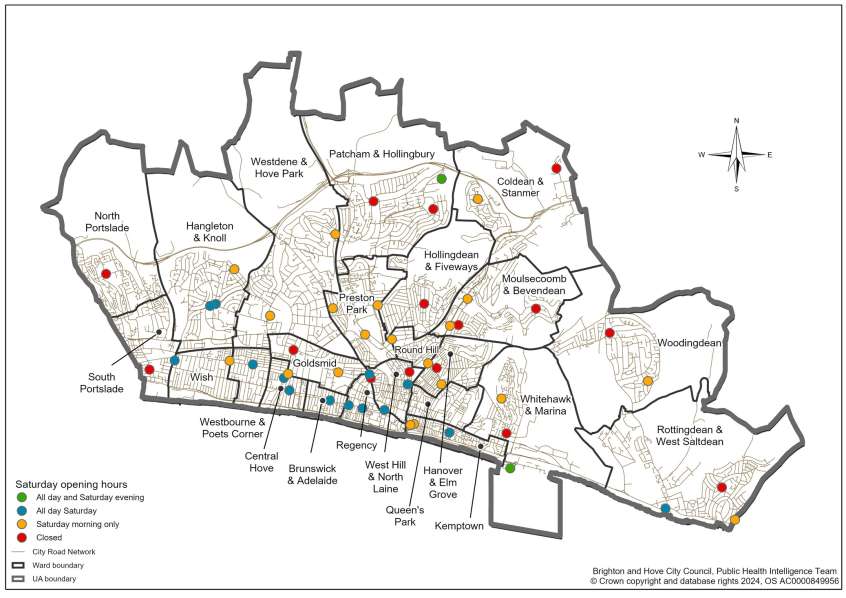
3.8.5 Routine Sunday daytime access to community pharmacies
Fewer pharmacies (4, 8%) are open on Sundays than on any other day in Brighton & Hove, which typically mirrors the availability of other healthcare providers open on a Sunday.
Full details of all pharmacies open on a Sunday can be found in Appendix A and in Figure 15 below.
Sunday opening is maintained in key central areas, ensuring continued access to pharmacy services.
Figure 15: Map of pharmacy opening hours in Brighton & Hove (Sunday)
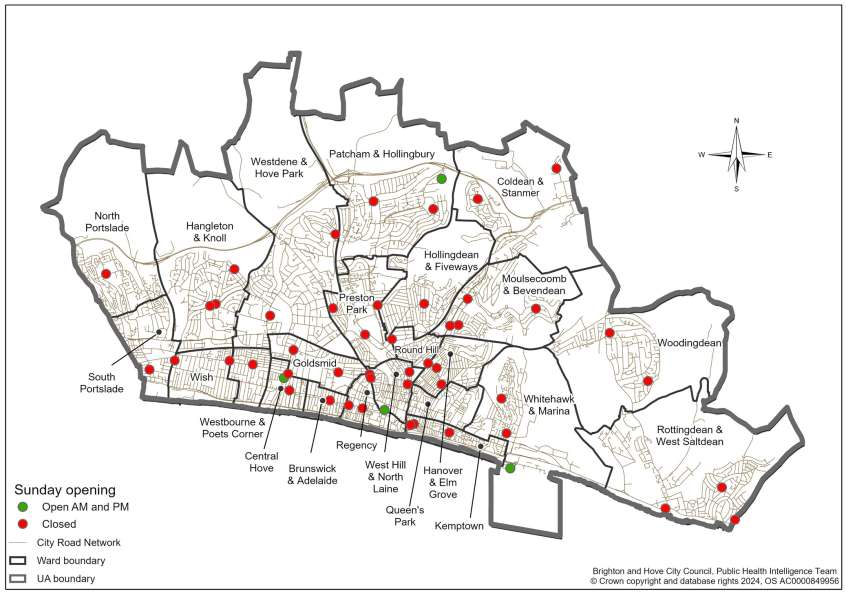
3.8.6 Routine bank holiday access to community pharmacies
Community pharmacies are not obliged to open on nominated bank holidays. While many opt to close, a number of pharmacies (often those in regional shopping centres, retail parks, supermarkets and major high streets) opt to open, often for limited hours.
The ICB has commissioned an Enhanced Service to provide coverage over Bank Holidays, Good Friday, Easter Sunday and Christmas Day, to ensure that there are pharmacies open on these days so patients can access services if required.
Details of which pharmacies are open can be found on the NHSE website.
3.9 Advanced Service provision from community pharmacy
Advanced Services look to ease the burden on other primary care services by providing access to healthcare professionals in a high street setting.
Section 1.5.5.2 lists all the Advanced Services that may be provided under the pharmacy contract.
As these services are discretionary, not all providers will provide them. Community pharmacies need to sign up to provide some of these services. In order to understand, provision data has been sourced by various methods to populate Table 13.
Data supplied from the ICB has been used to demonstrate how many community pharmacies per district have signed up to provide the Advanced Services, and data from the NHS Business Services Authority (NHS BSA claims from dispensing activities September to November 2024) demonstrates whether the service has been provided, based on pharmacies claiming payment.
Details of individual pharmacy providers can be seen in Appendix A.
It should be noted that for some services, such as AUR and SAC, provision is recorded as low through community pharmacies, as DACs (a specialised supplier of medical appliances and devices) provide these services.
Table 13: Summary of Advanced and Enhanced Service provision in Brighton & Hove
| Service | Brighton & Hove |
|---|---|
| Pharmacy First | 98% (94%) |
| Flu vaccination service | N/A (92%) |
| Pharmacy Contraception Service (PCS) | 80% (71%) |
| Hypertension Case Finding Service | 92% (82%) |
| New Medicine Service (NMS) | 96% (94%) |
| Smoking Cessation Service (SCS) | 73% (6%) |
| Appliance Use Review (AUR)* | N/A (0%) |
| Stoma Appliance Customisation (SAC)* | N/A (0%) |
| Lateral Flow Device (LFD) test supply service | 76% (51%) |
| COVID-19 vaccination service** | 49% (N/A) |
| Bank Holiday service*** | 14% (N/A) |
Note: The numbers in the table represent the percentage of providers who have signed up to the service, where information is available, and in brackets those that have claimed payment for service between September and November 2024.
*This service is typically provided by the DACs.
**At the time of writing, the service had only just restarted and therefore no activity data. This does not reflect the provision due to the seasonal trend in activity.
***This is correct at the time of writing; however, any pharmacy may apply to open or be directed to open depending on need. It may also not be the same pharmacies on each bank holiday.
Newer Advanced Services are increasing in activity based on the details provided in the 2022 PNA.
The Hypertension Case-finding Service has increased uptake from 60% to 92%; NMS from 67% to 96% and the Smoking Cessation Service, although currently providing few consultations at local and national level, 73% pharmacies are signed up in Brighton & Hove, a notable increase from the 4% recorded in 2022.
The low consultation number is also due to this service relying on a referral from secondary care.
3.10 Enhanced Service provision from community pharmacy
There is currently one National Enhanced Service commissioned through community pharmacies from the NHSE in Brighton & Hove. This is the COVID-19 vaccination service. In Brighton & Hove, 25 pharmacies (49%) are signed up to provide this service, as shown in Table 13 above. This is a significant increase from 8% in 2022.
The Bank Holiday opening service is a Local Enhanced Service, and 7 pharmacies (14%) were signed up to open on the Easter bank holiday 2025.
Any Locally Commissioned Services (LCS) commissioned by the ICB or the local authority are not considered here. They are outside the scope of the PNA but are considered in Section 4.
Section 4: Other services that may impact on pharmaceutical services provision
Community pharmacies and GP practices provide a range of other services. These are not considered ‘pharmaceutical services’ under the PLPS Regulations and may be either free of charge, privately funded or commissioned by the local authority or ICB.
These services are listed for information only and would not be considered as part of a market entry determination.
Examples of such services include delivery services, allergy testing, care home services and sexual health services, although this is not an exhaustive list.
Some of these services are also not exclusive to community pharmacies and are often commissioned through a range of providers.
A summary of the services commissioned is detailed below.
4.1 Integrated Care Board (ICB) - commissioned Services
The Sussex ICB commissions 3 services across Brighton & Hove. A summary of providers is listed in Table 14, and the full list of services provided by each community pharmacy can be found in Appendix A.
Table 14: Providers for Sussex ICB commissioned services in Brighton & Hove
| ICB-commissioned Service (ICBS) | Number (%) of pharmacies |
|---|---|
| ICBS1: Palliative care (end of life) | 9 (18%) |
| ICBS2: Supply of oral antiviral medication for COVID-19 and Influenza | 1 (2%) |
Sussex ICB is also part of the NHSE Independent Prescribing Pathfinder Programme, which funds the service in 2 sites across the ICB, but neither is in Brighton & Hove.
4.2 Local Authority-commissioned Services (LAS) provided by community pharmacies in Brighton & Hove
Brighton & Hove City Council (BHCC) commissions 10 services from community pharmacies in Brighton & Hove. These services may also be provided by other providers, for example, GP practices and community health services.
A summary of services and the total number of pharmacy providers (excluding the DSP) is listed below in Table 15, and the full list of services each community pharmacy provides can be found in Appendix A.
These locally commissioned services have been commissioned in Brighton & Hove based on the city’s specific population needs, public health challenges, and health inequalities.
Each service directly supports local health priorities, as identified in the:
- PNA
- JSNA
- NHS Sussex Integrated Care Strategy
Table 15: Providers for Brighton & Hove City Council (BHCC) commissioned services in Brighton & Hove
| Local Authority-commissioned Service | Number (%) of pharmacies |
|---|---|
| LAS1: Sexual health service: Emergency Hormonal Contraception (EHC) | 35 (70%) |
| LAS2: Sexual health service: Chlamydia screening and treatment | 23 (46%) |
| LAS3: Stop smoking: Adults scheme | 26 (52%) |
| LAS4: Stop smoking: Young people | 19 (38%) |
| LAS5: Stop smoking: Domiciliary care | 11 (22%) |
| LAS6: Stop smoking: Nicotine Replacement Therapy (NRT) voucher | 29 (58%) |
| LAS7: Healthy Living Pharmacy (HLP) campaigns and Alcohol brief intervention will be decommissioned from 1 April 2025 | 40 (80%) |
| LAS8: Substance misuse service: Naloxone provision | 20 (40%) |
| LAS9: Substance misuse service: Supervised consumption | 45 (90%) |
| LAS10: Substance misuse service: Needle and syringe exchange | 13 (26%) |
These services are listed for information only and would not be considered or used as part of a market entry determination.
4.3 Other services provided by community pharmacies
4.3.1 Collection and delivery services
The delivery services offered by pharmacy contractors are not commissioned services and are not part of the community pharmacy contractual terms of service. This is an unfunded service. This would not be considered as part of a determination for market entry.
Free delivery is required to be offered without restriction by all DSPs to patients who request it throughout England.
There is one DSP based in Brighton & Hove, and there are 409 throughout England.
Free delivery of appliances is also offered by DACs, and there are 112 DACs throughout England.
4.3.2 Services for less-abled people
Under the Equality Act 2010, community pharmacies are required to make ‘reasonable adjustments’ to their services to ensure they are accessible to all groups, including less-abled persons.
Of the 358 responders to the public questionnaire, 63% have identified that they have a disability. When asked if their ability to carry out day-to-day activities was reduced, 95 respondents (27%) stated a little and 50 (14%) answered that it was reduced a lot. From the same survey, 45 respondents (9%) stated their activities were limited by a physical difference.
Only 3% responded to the survey to say they chose a pharmacy based on disabled access.
4.4 Other providers
The following are providers of pharmacy services in Brighton & Hove, but are not defined as pharmaceutical services under the PLPS Regulations; however, they reduce the need for pharmaceutical service provision, in particular, the dispensing service.
4.4.1 NHS hospitals
- University Hospitals Sussex NHS Trust
- Sussex Community NHS Foundation Trust
- Sussex Partnership NHS Foundation Trust
4.4.2 Personal administration of items by GP practices
GPs can personally administer certain items, such as vaccines and certain injectable medications, for reimbursement from the NHS.
4.4.3 Flu vaccination service by GP practices
GP practices provide access to flu vaccination in addition to the service commissioned in pharmacies through their NHS Enhanced service.
4.4.4 Substance misuse services
There are a number of treatment and support providers for stopping and reducing smoking and alcohol in Brighton & Hove, including:
- Change Grow Live: Richmond House, Richmond Road, Brighton BN2 3FT
- Oasis Project: 11 Richmond Place, Brighton BN2 9NA
- Healthy Lifestyles Team
4.5 Other service providers
The following services may increase the demand for pharmaceutical service provision.
4.5.1 Urgent care centres
There is a walk-in centre within the Brighton Station Health Centre: Brighton Station Health Centre, Aspect House, 84-87 Queens Road, BN1 3XE.
Residents also have access to an urgent treatment centre at Lewes Victoria Hospital: Lewes Victoria Hospital, Nevill Road, Lewes, BN7 1NP.
4.5.2 Extended hours provided by Primary Care Networks (PCNs)
PCNs are required to provide enhanced access to appointments outside of the standard opening hours, for most GPs to accommodate those who may need appointments outside typical opening/working hours.
4.5.3 Community nursing prescribing
Community nurses work in a variety of settings, providing care to individuals outside of a normal acute or general practice setting. This can range from community-based clinics offering specialist services to directly visiting patients in their homes.
4.5.4 Dental services
Dentists can prescribe through their dental practices and may issue prescriptions for their patients when necessary.
4.5.5 End of life services
Palliative care services are provided by other providers such as hospices and specialist nurses.
4.5.6 Sexual health centres
Brighton sexual health and contraception services are available from various locations:
- SHAC West: Wish Park Surgery, 191 Portland Road, Hove, BN3 5JA
- SHAC Central: Morley Street, Brighton, BN2 9RE
- SHAC East: Claude Nicol Centre, Outpatients Department, Eastern Road, Brighton, BN2 5BE
- HIV Outpatients: The Lawson Unit, Louisa Martindale Building, Royal Sussex County Hospital, Eastern Road, Brighton, BN2 5BE
- Clinical Research Facility: Sussex House, 1 Abbey Road, Brighton, BN2 1ES
4.6 Other services
The following are services provided by NHS pharmaceutical providers in Brighton & Hove, commissioned by organisations other than NHSE or provided privately, and therefore out of scope of the PNA.
Privately provided services
most pharmacy contractors and DACs will provide services by private arrangement between the pharmacy or DAC and the customer or patient.
The following are examples of services and may fall within the definition of an Enhanced Service. However, as the service has not been commissioned by the NHS and is funded and provided privately, it's not a pharmaceutical service:
- care home service, such as direct supply of medicines/appliances and support for medicines management services to privately run care homes
- Patient Group Direction (PGD) service, such as hair loss therapy, and travel clinics
- screening service, such as screening for skin cancer
Services will vary between providers and are occasionally provided free of charge, such as home delivery.
A private pharmacy in Brighton & Hove is Pharm@Sea, located in Royal Sussex County Hospital, Eastern Road, Brighton (BN2 5BE). It dispenses hospital-only outpatient prescriptions generated from within the hospital. It's a private pharmacy separate from the hospital's in-house pharmacy.
Section 5: Findings from the public questionnaire
A public questionnaire about pharmacy provision was developed by the steering group to understand the views of the public in Brighton & Hove. This survey is designed to understand how, why and when the residents use pharmaceutical services in Brighton & Hove.
The survey was made available online electronically through the Brighton & Hove City Council consultations website page, with paper and easy-read versions made available on request.
The survey was available online between 24 October and 30 December 2024.
While the survey findings are informative, they are based on a self-selected sample. This means that members of the public who chose to respond could be more likely to have a particular interest or experience with pharmacy services, which may not reflect the views of the wider population.
As such, the results are not statistically representative of all residents in Brighton & Hove and should be interpreted with some caution.
However, the survey was intentionally promoted through a broad range of communication channels to encourage diverse participation, including:
- social media channels
- posters were displayed in Brighton & Hove community pharmacies and local libraries
- digital posters were displayed on screens in public buildings and waiting rooms
- the Brighton & Hove City Council network, including the residents' newsletter and distribution among staff
- Healthwatch Brighton & Hove network, including newsletter and distribution of paper copies during events
- Sussex ICB network
- Sussex Interpreting Services, including promotion within their network and preparation of translated instructions and surveys for users who do not have English as their first language
Although demographic representation could not be controlled due to the open-access nature of the survey, concerted efforts were made to reach a wide audience. The findings, therefore, provide valuable insight into community experience and can be used to highlight areas that may require further investigation or targeted engagement.
There were 358 responses, including 4 responses from a paper version and 354 online, from a population of approximately 279,600 (0.13%) (mid-year estimate 2023), so the findings should be interpreted with some care regarding the representation of the community as a whole.
It should also be noted that the demographics of respondents do not fully reflect population demographics, with not all groups adequately represented, limiting how generalisable the findings are. A full report of the results can be found in Appendix D.
The way the survey was conducted and the questions asked were not the same as the previous PNA; however, where possible, a comparison is noted below.
5.1 Demographic analysis
Female respondents were 72%, compared to 24% male respondents.
The majority answering the survey were aged between 55 to 64 (23%), 45 to 54 (22%) and 65 to 74 (20%).
64% reported having a disability or long-standing illness.
The majority of the respondents came from a White British background (76%), with 7% from other White backgrounds, and the remaining from Black and Racially Minoritised backgrounds.
5.2 Visiting a pharmacy
87% had a regular or preferred local community pharmacy.
Most of the respondents (35%) visited a pharmacy a few times a month, which was similar to 2022 (40%).
33% said they do not have a preference for any particular time of day.
36% said the most convenient day typically varied.
78% have not used a pharmacy on a bank holiday in the last 12 months.
2% said they only used an online pharmacy, and 4% combined traditional and internet pharmacies.
5.3 Reason for visiting a pharmacy
The main reason for visiting a pharmacy for most (87%) was to collect prescriptions for themselves.
58% visited to buy medicines over the counter.
40% went to use a pharmacy service, and a further 40% to get advice from a pharmacist.
5.4 Choosing a pharmacy
The factors that most influenced the respondents in their choice of pharmacy were:
- near my home: selected by 85% of respondents
- opening hours: 33% of respondents
- near my local GP practice: 30% of respondents
- pharmacy available on the internet, disabled access, and staff available to talk in other languages were selected by only 4%, 3% and 3% of the respondents, respectively
- when asked if they use a pharmacy further away than the closest pharmacy available, 26% responded that they do, the reasons being easier access, parking availability, friendliness and helpfulness of staff and availability of additional services
5.5 Access to a pharmacy
The main way respondents access a pharmacy is by walking, with 60% using this method. The next most common method is to use a car (24%), followed by public transport (6%). These numbers were similar to how individuals answered in 2022, with 54% walking, 29% using a car and 9% using public transport.
Of respondents, 91% reported that they were able to travel to a pharmacy in less than 20 minutes, and only 2% needed more than 30 minutes to get to their chosen pharmacy.
5.6 Other comments
Members of the public were asked to provide any further comments regarding pharmacy services across Brighton & Hove. Below are the key themes collated with further details in Appendix D.
Hours
While most respondents found pharmacy opening hours met their needs, 25 (7%) suggested that extending late-night, weekend, and bank holiday services would provide additional benefits for the community.
21 (6%) respondents highlighted that enhanced availability outside standard working hours could particularly support full-time workers.
14 (4%) noted that extended opening, including beyond lunchtime and on Saturday afternoons, would further improve access.
Access
General access across Brighton & Hove was viewed positively by many respondents.
However, 13 participants identified opportunities to strengthen access in specific areas, particularly Kemptown and Rottingdean.
8 reported accessibility issues, including a lack of disabled parking and difficulties faced by elderly users, such as navigating online services.
Service
Pharmacy staff were widely praised, with 15 (4%) highlighting their friendly, professional, and supportive approach.
Medication supply
12 (3%) reported difficulties sourcing medications, often having to visit multiple pharmacies. To note, this is a national issue and outside of the scope of the PNA process.
Other
15 (4%) participants expressed a concern about the reduction in the number of local pharmacies through closures.
Section 6: Analysis of health needs and pharmaceutical service provision
The purpose of this section is to provide an analysis of health needs and pharmaceutical service provision to establish if there is a gap or potential future gap in the provision of pharmaceutical services in Brighton & Hove in the next 3 years.
It also takes into consideration the priorities outlined in the NHS Long Term Plan, JSNA, JHWS, and other local policies and strategies.
Understanding the communities that local pharmacies serve is important for maximising national Community Pharmacy Contractual Framework (CPCF) services in care pathways, as well as commissioning the services that best serve the health and well-being requirements of the local communities.
Pharmacies play more than a medicine-dispensing role today, and the changes in the 2019 to 2024 CPCF saw services that meet the prevention, medicines optimisation and primary care access agendas.
6.1 Brighton & Hove current and future health needs
The future health needs of the population of Brighton & Hove will continue to change as the population lives longer. The council modelled estimates for the housing planning to 2033 project an increase of around 6,700 people (a 2.4% increase).
Numbers of older people in the age groups 65 to 84 and 85 plus are predicted to increase the most, with only the number of school-aged children predicted to decrease (source).
A consequence of more people living longer is an increased risk of dementia. In March 2020, there were 1,781 registered patients with dementia in the city (4.2% of residents 65 years or over). In Brighton & Hove in 2024, of those aged 65 and over, 65.9% had been diagnosed with dementia. This is similar to the national rate of 66.7% of the estimated population of people with dementia receiving a recorded diagnosis (source).
Over a third of older people in Brighton & Hove live alone, with 13,875 residents aged 65 and above (38%) living alone. This figure is significantly higher than the South East (30%) and England (31%), and is likely to increase if the number of residents in the age group 65 plus continues to increase. Living alone in later life is a risk factor for loneliness and isolation (source).
As people live longer, the proportion living with multiple long-term conditions requiring medication will also increase. People aged 65 to 69 years have, on average, 2 long-term conditions (LTCs), increasing to 3 by age 80 to 84 years.
The prevalence of long-term conditions among adults with multiple conditions is approximately 3 times higher than in the general adult population. Patients with Chronic Obstructive Pulmonary Disease (COPD) and Coronary Heart Disease (CHD) all have, on average, 3 other long-term conditions (source).
In 2022 to 2023, the prevalence rate for adult obesity in Brighton & Hove was 57.3%. This is lower than the England average of 64%. The trend in Brighton & Hove is improving, with prevalence down from 59.4% (source). However, with over one in two adults being overweight or experiencing obesity, it's important to continue all efforts to reduce this figure further, as it's a significant risk factor for:
- type 2 diabetes
- a number of cancers
- cardiovascular disease
- joint problems
Community pharmacies have an important role to play in both supporting individual behaviour change and the city’s whole systems approach to healthy weight, with an opportunity to offer advice and signpost to many local supports to get more active and maintain a healthy weight.
Nearly one in 10 of Brighton & Hove's total population (9%, 26,200 people) is aged 19 to 22 years old, compared to only 4% in the South East and 5% in England. This is related to the student population, as for the academic year 2021 to 2022, there were 37,700 students at the University of Sussex and the University of Brighton. This was an increase of 1.3% (500 students) compared to 2020 to 2021 (source).
In 2023, Brighton & Hove had the 14th highest rate of new Sexually Transmitted Infections (STIs) of all 152 English upper-tier local authorities (source). The emergency contraception service includes the free distribution of condoms via the C-card scheme to prevent sexually transmitted infections, and selected pharmacies also offer a chlamydia treatment service.
Other future health needs include cancer, alcohol and substance misuse.
Smoking prevalence in adults at 17.6% is significantly higher than in East Sussex at 12.5% and West Sussex at 11.3%, with a higher prevalence in adults in routine and manual occupations (19.5%) (source).
Community pharmacies continue to play a pivotal role in reducing smoking rates by offering stop smoking services and referrals, and domiciliary stop smoking services for housebound residents via the public health locally commissioned services.
Alcohol and drug misuse continue to be significant issues for the city. The city has a significantly higher rate of alcohol-specific mortality compared to England at 21.8 per 100,000 people, which is more than double the rate in England (5.2 per 100,000) (2020 to 2022) (source).
The city has a significantly higher drug-related death rate than England (source), as well as higher than average use of opiates and crack amongst adults.
Public health, in collaboration with the multiagency Combatting Drugs Partnership, has developed the Reducing Harm from Drugs and Alcohol Strategy 2024 to 2030.
Vaccination is one of the most effective public health interventions (source).
6.2 Pharmaceutical service provision
There are 51 community pharmacy contractors across Brighton & Hove who provide a range of services as part of the contractual obligations and a number voluntarily, commissioned either through NHSE as Advanced or Enhanced Services or through local commissioners based on local needs.
The Advanced and Enhanced Services support the needs of alleviating the burden on other primary care services and improving access.
With an ageing population, these services:
- support by helping older residents to manage their long-term conditions
- reduce hospital admissions by early intervention and prevention
- improve quality of life
The locally commissioned services support the specific local needs and public health challenges and help address health inequalities. They target the needs to address the conception rates, STIs, smoking rates and substance misuse across Brighton & Hove, as community pharmacies are highly accessible and feel less formal than other healthcare settings.
Community pharmacies are often found in areas of high deprivation and allow for ease of access in these areas and making services more accessible.
6.3 NHS pharmaceutical service provision for Brighton & Hove
As discussed in Section 1.4, NHS pharmaceutical services are considered for this PNA, as defined by the NHS PLPS Regulations 2013. For the PNA, all Essential Services are to be regarded as Necessary Services in Brighton & Hove.
Advanced Services (excluding Smoking Cessation Service, Appliance Use Review and Stoma Appliance Customisation Service) and Enhanced Services are considered as other relevant services for the 2025 PNA.
Locally commissioned services are noted within the PNA in Section 4 as other services; however, it's important to note that the absence of a service does not result in a gap, as often these services and needs are met by other providers. These are not used to determine market entry and, therefore, are outside of the scope of the PNA.
The breakdown of Advanced and Enhanced Service provision can be found in Sections 3.9 and 3.10.
For the PNA, Brighton & Hove has been considered as a single locality.
6.3.1 Necessary Services: essential services, current provision
Brighton & Hove has an estimated population of 279,600.
There are 51 community pharmacies (including one DSP) in Brighton & Hove. The estimated average number of community pharmacies per 100,000 population is 18.2, which is slightly higher than the England average of 18.1 and also higher than the rate of 17.8 in Brighton & Hove in the previous PNA (Section 3.2).
Of the 51 pharmacies:
- 50 (98%) pharmacies hold a standard 40 core hour contract
- one (2%) is a DSP
There are no DACs; however, these services can be provided by contractors outside of the area. There were no DACs in Brighton & Hove in the previously published 2022 PNA.
There are also no dispensing practices in Brighton & Hove.
Evening access
Although a small proportion of respondents (11%) expressed a desire for greater access after 6 pm, analysis shows that 18 pharmacies (35%) are open beyond 6 pm on a weekday, and 2 open until 8 pm. This ensures that evening access is maintained across the city.
Weekend and bank holiday access
36 (71%) pharmacies are open on Saturdays, providing substantial weekend access. Although fewer pharmacies open on Sundays, this pattern is consistent with national trends and other healthcare access.
Parking and physical accessibility
Concerns raised about parking and disabled access are addressed through mapping and local data. See Figure 9 in Section 3.8.1.2, which shows that the majority of pharmacies are located close to disabled parking bays.
Patients also have access to the DSP in Brighton & Hove and other DSPs in England, which have to deliver nationally as part of their contractual agreement.
There are also a number of accessible providers open in the neighbouring HWB areas of East Sussex to the east and West Sussex to the west.
6.3.2 Necessary Services: gaps in provision across Brighton & Hove
When assessing the provision of pharmaceutical services in Brighton & Hove, the steering group considered the following to understand the needs of the population:
- national and local priorities (Section 2).
- population changes and housing developments across the next 3 years (Section 2.7.2 and 2.7.3)
- IMD and deprivation ranges compared with the relative location of pharmacy premises (Section 2.7.4 and Figure 7 in Section 3.8)
- the burden of diseases and the lifestyle choices people make across Brighton & Hove (Sections 2.8 and 2.9)
- the health profiles based on ONS and QOF data (Sections 2.8 and 2.9)
The following have been considered to understand pharmaceutical service provision and access:
- the number and location of pharmacy contractors across Brighton & Hove and the neighbouring HWBs (Section 3.1)
- the ratio of community pharmacies per 100,000 and noting it's similar to the current England average (Section 3.2)
- what choice do individuals have to which pharmacy they choose to visit, including disabled parking spots (Section 3.8)
- how long it takes to travel to the nearest pharmacy based on various transportation methods (Section 3.8.1)
- weekend and evening access (Section 3.8.2)
- what services are provided (Sections 3.9 and 3.10) – note that every community pharmacy needs to provide essential services as part of the Community Pharmacy Contractual Framework.
- the views of the public on pharmaceutical service provision (Section 5)
Based on the mapped evidence, survey feedback, and local intelligence, there is good access to the Essential Services across Brighton & Hove. The ratio of community pharmacies per 100,000 is similar to the levels across England.
Travel analysis showed:
- 100% of the population who have access to a vehicle in Brighton & Hove can get to a pharmacy within 10 minutes by private transport
- 98.1% of the population who can walk can get to the nearest pharmacy within 20 minutes
- 100% have access to a pharmacy within a 20-minute journey by public transport
Individuals are able to travel to a pharmacy within reasonable times, although it may take longer for some residents in less populated areas; however, this would be no different to accessing other healthcare services or out-of-hours services in person.
Future provision
The current community pharmacy network across Brighton & Hove is adequate to meet the predicted population and housing growth across Brighton & Hove up to 2028. No new or future gaps in provision have been identified as a result of planned developments during the lifetime of this PNA.
While pharmacies, particularly sole providers, may experience increased footfall and service pressures, the network is resilient. Community pharmacies are well-placed to manage increased demand through adjustments to staffing, service models, and opening patterns where necessary, with no disruption to service provision anticipated.
By the time the PNA is published, a community pharmacy in Rottingdean is due to be removed from the pharmaceutical list. Although it has been closed for more than 6 months at the time of writing, March 2025, it remains on the list and has been included as part of this assessment.
• Rottingdean Pharmacy: 2 to 4 West Street, Rottingdean, Brighton, BN2 7HP.
When the pharmacy originally closed, several complaints were received; however, there have been no complaints since August 2024, and no evidence has been presented of any unmet need in the local area.
There would not be a pharmacy open within the vicinity all day on a Saturday, but there would be access to a pharmacy during Saturday morning.
The community pharmacy is not in an area of high deprivation or high population density.
When considering physical access to the nearest pharmacy, residents are able to travel and access within 20 minutes, regardless of the transportation method chosen.
A comparison of before and after is shown in the table below.
Table 16: Comparison of travel time to pharmacy in Brighton & Hove before and after closure of Rottingdean pharmacy
| Transport method | Time (including Rottingdean) | Population within time band (including Rottingdean) | Time (without Rottingdean) | Population within time band (without Rottingdean) |
|---|---|---|---|---|
| Car (not rush hour) | 10 minutes | 278,370 (100%) | 10 minutes | 278,370 (100%) |
| Walk | 10 minutes | 234,522 (84.2%) | 10 minutes | 232,779 (83.6%) |
| Walk | 20 minutes | 272,947 (98.1%) | 20 minutes | 271,204 (97.4%) |
| Public transport (weekday morning) | 10 minutes | 275,535 (99%) | 10 minutes | 275,535 (99%) |
| Public transport (weekday morning) | 20 minutes | 278,370 (100%) | 20 minutes | 278,370 (100%) |
After the closure of the pharmacy, residents in Brighton & Hove are still able to travel to a pharmacy within a reasonable time, although it may take longer for some residents on the outskirts, such as the South East; however, this would be no different to accessing other healthcare services or out-of-hours services in person.
Based on this assessment, there is no gap as a result of this closure.
There are no gaps in the provision of Necessary Services at present or in the future (next 3 years) across Brighton & Hove.
6.3.3 Other relevant services: current provision
Advanced and Enhanced Services look to ease the burden on other primary care services by providing access to a healthcare professional in a high street setting; however, the absence of a service due to a community pharmacy signing up does not result in a gap.
Table 13 in Section 3.9 shows the pharmacies providing Advanced and Enhanced Services in the Brighton & Hove HWB area.
Regarding access to Advanced services, it can be seen that there is very good availability of Pharmacy First (98%), NMS (96%), Flu Vaccination (92%), Hypertension Case-finding (92%) and PCS (80%).
There is also good availability of LFD test supplies (76%).
Regarding access to National Enhanced Services, 25 pharmacies (49%) offer the COVID-19 vaccination service, and 7 (14%) are open on bank holidays.
Consideration should be given to incentives for further uptake from current providers and extending provision through community pharmacies, including plans to increase uptake of the service through existing providers working with place-based stakeholders.
The DSP in Brighton & Hove currently provides COVID-19 vaccination. The DSP does not provide any Advanced or Locally Commissioned Services and cannot provide Essential Services face-to-face. With the upcoming change in regulations, DSPs will no longer be able to provide face-to-face services.
There are no gaps in the provision of other relevant services at present or in the future (next three years) across Brighton & Hove.
6.4 Improvements and better access: gaps in provision across Brighton & Hove
Regarding access to services commissioned by Sussex ICB, see Table 17.
Table 17: Providers for Sussex ICB commissioned services in Brighton & Hove
| Service | Number (%) of pharmacies |
|---|---|
| Palliative care (end of life) | 9 (18%) |
| Supply of oral antiviral medication for COVID-19 and Influenza | 1 (2%) |
| Bank holiday service | 7 (14%) |
Regarding access to services commissioned by BHCC, see Table 18.
Table 18: Providers for BHCC commissioned services in Brighton & Hove
| Service | Number (%) of pharmacies |
|---|---|
| Sexual health service: EHC | 35 (70%) |
| Sexual health service: Chlamydia screening and treatment | 23 (46%) |
| Stop smoking- Adults | 26 (52%) |
| Stop smoking - Young people | 19 (38%) |
| Stop smoking - Domiciliary care | 11 (22%) |
| Stop smoking - NRT voucher | 29 (58%) |
| HLP campaigns and Alcohol brief Intervention | 40 (80%) |
| Substance misuse service: Naloxone provision | 20 (40%) |
| Substance misuse service: Supervised consumption | 45 (90%) |
| Substance misuse service: Needle and syringe exchange | 13 (26%) |
All locally commissioned services are available in Brighton & Hove and have varying opening times. As these are not NHS commissioned services, they are out of scope of the assessment; however provide access to local residents to a number of needs across the area.
No gaps have been identified in either the necessary services or any other relevant services that, if provided either now or in the future (next 3 years), would secure improvements or better access to the Essential or specified Advanced and Enhanced services across Brighton & Hove.
Section 7: Conclusions
The Steering Group provides the following conclusions on the basis that funding is at least maintained at current levels and/or reflects future population changes.
There is a wide range of pharmaceutical services provided in Brighton & Hove to meet the health needs of the population. The provision of current pharmaceutical services and LCS are distributed across localities, providing good access throughout Brighton & Hove.
As part of this assessment, no gaps have been identified in provision either now or in the future (over the next 3 years) for pharmaceutical services deemed Necessary.
7.1 Statements of the PNA
The PNA is required to clearly state what is considered to constitute Necessary Services as required by paragraphs 1 and 3 of Schedule 1 to the PLPS Regulations.
For this PNA, Essential Services for Brighton & Hove HWB are to be regarded as Necessary Services.
Other Advanced (apart from SCS, AUR and SAC) and National Enhanced Services are considered relevant as they contribute toward improvement in provision and access to pharmaceutical services.
Locally commissioned services are those services that secure improvements or better access to, or which have contributed towards meeting the need for, pharmaceutical services in Brighton & Hove HWB areas, and are commissioned by the ICB or local authority, rather than NHSE.
7.1.1 Current provision of Necessary Services
Necessary Services – gaps in provision
Essential services are Necessary Services, which are described in Section 1.5.5.1. Access to Necessary Service provision in Brighton & Hove is provided in Section 6.
In reference to Section 6, and required by paragraph 2 of Schedule 1 of the PLPS Regulations:
Necessary Services – normal working hours
There is no gap in the provision of Necessary Services during normal working hours across Brighton & Hove to meet the needs of the population.
Necessary Services – outside normal working hours
There are no gaps in the provision of Necessary Services outside normal working hours across Brighton & Hove to meet the needs of the population.
7.1.2 Future provision of Necessary Services
No gaps have been identified in the need for pharmaceutical services in specified future (next 3 years) circumstances across Brighton & Hove.
7.1.3 Other relevant services - gaps in provision
Advanced Services (apart from SCS, AUR and SAC) and the National Enhanced Service are considered relevant as they contribute toward improvement in provision and access to pharmaceutical services.
7.1.3.1 Current and future access to Advanced Services
Details of the Advanced Services are outlined in Section 1.5.5.2, and the provision in Brighton & Hove is discussed in Sections 3.9 and 6.3.3.
Section 6.4 discusses improvements and better access to services in relation to the health needs of Brighton & Hove.
Based on the information available at the time of developing this PNA, no gaps in the current provision of Advanced Services or in specified future (next 3 years) circumstances have been identified in any of the localities across Brighton & Hove.
Section 9 discusses the opportunities that may be available for expansion of existing services or delivery of new services from community pharmacies that may benefit the population of Brighton & Hove.
There are no gaps in the provision of Advanced Services at present or in the future (next 3 years) that would secure improvements or better access to services in Brighton & Hove.
7.1.3.2 Current and future access to Enhanced Services
Details of the National Enhanced Service are outlined in Section 1.5.5.3, and the provision in Brighton & Hove is discussed in Sections 3.10 and 6.3.3.
Section 6.4 discusses improvements and better access to services in relation to the health needs of Brighton & Hove.
Based on the information available at the time of developing this PNA, no gaps in the current provision of National Enhanced Services or in specified future (next 3 years) circumstances have been identified in any of the localities across Brighton & Hove.
No gaps have been identified that if provided either now or in the future (next 3 years) would secure improvements or better access to National Enhanced Services across Brighton & Hove.
7.1.3.3 Current and future access to Locally Commissioned Services (LCS)
With regard to LCS, the PNA is mindful that only those commissioned by NHSE are regarded as pharmaceutical services.
The absence of a particular service being commissioned by NHSE is, in some cases, addressed by a service being commissioned through the ICB or the local authority; these services are described in Sections 4.1 and 4.2.
Section 6.4 discusses improvements and better access to LCS in relation to the health needs of Brighton & Hove.
Based on the information available at the time of developing this PNA, no gaps have been identified in LCS that, if provided either now or in the future (next 3 years), would secure improvements or better access in any of the localities.
Future improvements and better access are best managed through working with existing contractors and improving integration with other services and within Primary Care Networks (PCN), rather than through the opening of additional pharmacies.
Based on current information, the Steering Group has not considered that any of these LCS should be decommissioned; however, the HWB and commissioning organisations may want to consider incentivising community pharmacies to encourage further uptake of services.
Section 9 discusses the opportunities that may be available for expansion of existing services or delivery of new services from existing community pharmacies that may benefit the population of Brighton & Hove.
A full analysis has not been conducted on which LCS might be of benefit, as this is out of the scope of the PNA.
7.1.4 Improvements and better access – gaps in provision
Based on current information, no gaps have been identified in respect of securing improvements or better access to other relevant services, either now or in specific future circumstances across Brighton & Hove to meet the needs of the population.
Section 8: Recommendations from the previous PNA: Status to date
A series of recommendations were made in the previous PNA, which, although they were out of scope of the PNA process, were seen as opportunities to enhance service provision across Brighton & Hove.
Below is a list of the recommendations and what actions were taken.
Vaccinations
- The Brighton & Hove Flu and Covid-19 Programme Board to consider how community pharmacies can work more closely with GP practices and others in offering and increasing the uptake of the NHS flu vaccination, particularly for staff and residents in care settings.
Community pharmacies offer a walk-in vaccination service and are included as an option on the national vaccination booking service and other booking portals. This is in addition to vaccines provided by GP practices.
The service specification also allows the administration of flu vaccines in other suitable locations, such as care homes for staff and residents.
The Brighton & Hove Flu and Covid-19 Programme Board has been dissolved; however, the move to neighbourhood teams will support closer working when planning flu vaccination in care settings for 2025 to 2026, particularly in the east of the city.
Recommendation completed.
- NHS England and NHS Sussex Integrated Care Board (ICB) to consider commissioning Pneumococcal Polysaccharide Vaccine (PPV) and shingles vaccinations via community pharmacy to maximise delivery alongside the flu vaccination in pharmacies and support increasing uptake.
The NHS vaccination strategy published in December 2023 mentions integrating vaccination into existing clinical pathways.
Responsibility for commissioning vaccination services will be delegated to ICBs in April 2026. There is an opportunity for engagement with the ICB to review additional vaccinations that could be delivered in the community pharmacy setting.
To date, NHS England has published an invitation to tender (ITT) inviting community pharmacy owners interested in providing a Community Pharmacy Respiratory Syncytial Virus (RSV) and Pertussis Vaccination Enhanced Service in the Midlands area.
Recommendation not completed: work is ongoing in this area, and there is an opportunity to increase vaccination uptake.
- NHS England and the Sussex ICB are to increase the number and geographical spread of community pharmacies delivering COVID-19 vaccinations. This is to increase access across the city and uptake of COVID-19 vaccinations (including uptake by children), as well as in response to high satisfaction with pharmacy services.
NHSE commissions an Enhanced Service: Covid-19 vaccination programme. This service is commissioned until 31 March 2026. At the time of writing, 24 pharmacies are providing the service in Brighton & Hove, which is a significant increase from the 4 pharmacies that were providing the service in 2022.
In terms of access, there is good provision in the west, central and north of the city, and satisfaction remains high; however, more provision is needed in the east, and this should be considered by commissioners when planning the COVID-19 2025 to 2026 programme from the existing pharmacies.
Recommendation completed.
Evening pharmacy provision
- Sussex Integrated Care Board / Integrated Care System and NHS England to review the commissioning and provision of evening pharmacy provision from current pharmacies beyond the existing provision after 8pm Monday to Wednesday and Saturday, after 9pm Thursday and Friday, and after 6pm on Sundays.
Two Asda pharmacies (Brighton Marina and Hollingbury) are open in the evening until 8pm, Monday to Saturday, but no pharmacies are open after 5 pm on a Sunday. The provision of evening services has reduced since 2022.
Recommendation completed: No gap identified as part of the 2025 PNA.
- Community pharmacy capacity to meet city needs: Public health commissioners to review opportunities for pharmacies that are open after 6pm on weekdays and at weekends to consider providing the emergency hormonal contraception service to improve accessibility in Brighton & Hove.
The public health commissioners reviewed the Sexual Health and Contraception service as recommended.
To increase accessibility to the service, community pharmacists can supply free emergency hormonal contraception over the counter according to the Pharmacy Medicine Regulations and claim the cost from public health via the locally commissioned service.
The service specification has been adapted to enable pharmacies that are open after 6pm and at weekends to offer the service for a reduced duration, provided the ‘out of hours’ times are included.
Emergency hormonal contraception will be added to the national pharmacy contraception service from October 2025 and will further increase access.
Recommendation completed.
- NHS England and the Sussex ICB to review pharmacy commissioning and capacity in areas with significant increases in future housing developments.
Despite increases in housing developments, for the period covered by this Pharmaceutical Needs Assessment, there is considered to be no gap in community pharmacy provision, but with a projected population increase, this should be kept under review.
There has been no gap identified with the projected population growth or housing projections within this PNA now or in the next 3 years.
Improving health and wellbeing
- Public health commissioners to review the provision of the stop smoking, young persons and domiciliary stop smoking services and to support community pharmacies to re-establish these services and encourage their uptake.
A new stop smoking service specification was developed in April 2023 to encourage Brighton & Hove residents to stop smoking. For the year ending 1 April 2025, the service has supported 145 people to stop smoking.
The service is being developed further in June 2025 to include 2 stop smoking medicines as alternative options to nicotine replacement therapy.
Recommendation completed.
- NHS England, the Sussex ICB and public health commissioners to ensure that stop smoking service pathways are joined up and communicated to people wishing to stop smoking. Other health/social care providers should be made aware of referral pathways into stop smoking services.
A community pharmacy stop smoking networking event was organised in February 2024 by the community pharmacy and public health forum to increase the awareness of the stop smoking pathways in Brighton & Hove and access points for Brighton & Hove residents.
This event included representatives from:
- the stop smoking services in University Hospital Sussex
- maternity services
- community pharmacy and GP practice providers
Recommendation completed.
- NHS England and the Sussex ICB to review the need for the community pharmacy Hepatitis C antibody testing service in Brighton & Hove, based on population health needs and commissioning of substance misuse services and to support increasing uptake.
In agreement with the Pharmaceutical Services Negotiating Committee and the Department of Health and Social Care (DHSC), NHS England decommissioned the national Community Pharmacy Hepatitis C Antibody Testing Service from 1 April 2023. The service aimed to increase the diagnosis of Hepatitis C and was part of the groundbreaking NHS initiative on Hepatitis C (source).
The NHS is indeed on track to eliminate Hepatitis C in England by 2025. This ambitious goal is being achieved through a combination of effective treatments, targeted testing, and a "find and treat" approach, especially for vulnerable communities.
Recommendation completed.
- The Community Pharmacy and Public Health Forum to increase participation of Brighton & Hove-commissioned Healthy Living Pharmacies in local health promotion campaigns and encourage increased signposting/referrals into related services such as weight management and drug and alcohol support.
29 pharmacies in Brighton & Hove are commissioned under the local Healthy Living Pharmacies programme, and they are contractually obliged to participate in 3 local Public Health campaigns per year.
Previous campaigns focused on health issues like cardiovascular disease and prevention measures such as reducing alcohol intake and smoking cessation.
The 2024 to 2025 calendar offered an opportunity to focus on ovarian cancer in September (which was Gynaecological Cancer Month) and renal cancer in February 2025.
Recommendation completed.
- Sussex ICB to deliver a communications and engagement campaign to increase utilisation of the newly commissioned Hypertension Case-finding Service and other new services in community pharmacies. Increasing communications and engagement will lead to an increase in the take-up of new services and an increase in the detection of hypertension, improving cardiovascular disease prevention in the city.
Since the relaunch of the Hypertension Case-finding Service in November 2023 as part of the 'Delivery plan for recovering access to primary care', further pharmacy contractors have signed up to provide the service, with 47 out of 50 (92%) in Brighton & Hove registered.
Since December 2023, over 48,000 consultations have taken place across Sussex.
NHS Sussex has been working with Community Pharmacy Surrey and Sussex, and with the Sussex ICB cardiovascular clinical lead, to encourage the use of this referral route from general practice for patients already diagnosed with hypertension.
Recommendation completed.
- Sussex ICB to look at the development and commissioning of new services to be delivered by community pharmacy that result in taking pressure off GP practices and urgent and emergency care. Part of this work is to review the case for developing a urinary tract infection service in community pharmacies in order to improve patient access and reduce pressure on urgent care pathways.
In January 2024, NHS England commissioned a new service, Pharmacy First (Section 1.2). This service enables patients to get certain prescription medications directly from a pharmacy where appropriate, without a GP appointment.
It includes the supply of appropriate medicines for 7 common conditions, including earache, sore throat, and urinary tract infections, aiming to address health issues before they get worse.
The uptake for this service is likely to increase, and it's being reviewed to include more conditions.
Equality of access to community pharmacy services
- Sussex ICB and NHS England to review the needs of residents with disabilities in accessing community pharmacy services in Brighton & Hove. This should build on the findings from the previous PNA (2018), include coverage of disabled parking bays near pharmacies, the need and affordability of a home delivery service for medicines, and adherence to the Public Sector Bodies (Websites and Mobile Applications) (No.2) Accessibility Regulations 2018.
A map of Brighton & Hove Pharmacies and the location of disabled parking bays has been included in the PNA 2025 (Figure 9). According to the NHS Terms of Service, pharmacy owners must verify and update their opening hours, contact details, facilities, and services information for each profile every financial quarter.
The NHS profile includes information about the availability of facilities such as ramps for wheelchair access and hearing loops, and services.
The General Pharmaceutical Council provides equality guidance for pharmacies according to the Equality Act 2010. It introduces the ‘duty to make reasonable adjustments’ to the property services provided, to meet the needs of disabled people, including employees. This may mean changing the way services are delivered.
Although a number of community pharmacies provide a medicine delivery service, this is not funded under the NHS contract.
Recommendation completed.
- Public health to ensure that the publication of the PNA report adheres to the Public Sector Bodies (Websites and Mobile Applications) (No.2) Accessibility Regulations 2018.
The Brighton & Hove Accessibility City Strategy 2023 to 2028 sets out how Brighton & Hove City Council ensures adherence to the Accessibility Regulations 2018.
Recommendation completed.
- Sussex ICB and NHS England to ensure that different methods of interactive services available in community pharmacies are available to people without internet access.
Organisations that provide NHS care, including community pharmacies, are legally required to follow the Accessible Information Standard.
The Standard sets out a specific, consistent approach to identifying, recording, flagging, sharing and meeting the information and communication support needs of patients, service users, carers and parents with a disability, impairment or sensory loss.
Community pharmacies are encouraged to demonstrate the principles by asking people about their communication or accessibility needs, providing information about accessibility and making reasonable adjustments to support people with, for example, medication labels in a larger font.
Recommendation completed.
- Sussex ICB and NHS England to ensure people with English language needs are aware of the interpreter/translation service available in the city, which is for use in any health and care setting, including community pharmacy.
All community pharmacies in Brighton & Hove have access to high-quality interpreting and translation services, which include:
- face-to-face, telephone and remote community language interpreting
- face-to-face, telephone and remote British Sign Language (BSL) interpreting (including Signlive on-demand BSL interpreting)
- translation services, including BSL videos, Braille and Easy Read
- bilingual advocacy
The service is provided by Sussex Interpreting Services, and community pharmacies can register for an account to enable access to the service. This information has been circulated to pharmacies via the Community Pharmacy Surrey and Sussex newsletters.
Recommendation completed.
Awareness and knowledge of services and facilities available in community pharmacies
- The Brighton & Hove Community Pharmacy and Public Health Forum to agree on how to improve GP practice knowledge of services in community pharmacies to increase signposting and referrals by GP practice staff to community pharmacies. This includes referrals for all essential, advanced and locally commissioned services.
The Community Pharmacy Surrey and Sussex members of the forum have led an initiative to increase awareness of services in community pharmacies. This has included a presentation to the Brighton GP Federation to update them on services available in pharmacies and how to refer to services.
Joint work with the Trust for Developing Communities has resulted in a flyer with a QR code detailing services for residents across Brighton & Hove and how to access them.
This work is ongoing and is reviewed regularly at the forum meetings.
- NHS Sussex ICB, NHS England, BHCC and East and West Sussex councils to work together to increase public understanding of community pharmacy provision to better communicate across boundaries pharmacy provision including health promotion and prevention services.
Public Health commissioned community pharmacy service specifications are shared across the 3 councils to share best practice and ways of working, and to avoid duplication of workstreams.
Stop smoking services for all 3 councils are being updated to ensure equitable access to stop smoking medicines across Sussex, with a plan to start in June 2025.
Recommendation not completed: work is ongoing in this area.
- NHS England to explore with NHS Digital the possibility of including a wider range of options on the Find My Pharmacy website, so that all services being provided at community pharmacies can be shown. Also, to ensure information about accessibility issues (for example, ramps and lifts) for disabled people is covered.
The Find My Pharmacy Website has been updated to include search options for NHS services provided by community pharmacies, such as:
- free flu vaccination
- free blood pressure checks
- contraception services
Refer to the recommendation above for accessibility information.
Recommendation completed.
- NHS England to ensure that community pharmacies keep pharmacy information on NHS websites up to date, in line with NHS Profile Manager guidance and Accessibility Standards 2018.
According to the NHS Terms of Service, pharmacy owners must verify and update their opening hours, contact details, facilities, and services information for each profile every financial quarter.
The service profile includes opening times, contact details, facilities and service information. This ensures accurate information for patients and NHS professionals.
Recommendation completed.
Cross-system working
- Sussex ICB and Brighton & Hove City Council to review how the Community Pharmacy and Public Health Forum fits with the new Sussex NHS structures and the integration of the commissioning of local pharmaceutical services, and ensure involvement of community pharmacy in the development of health and wellbeing strategic plans.
The Community Pharmacy and Public Health Forum encourage and supports collaborative working between the Brighton & Hove City Council Public Health team, NHS Sussex, Brighton & Hove PCNs, Community Pharmacy Surrey and Sussex and other partnership groups, including patient participation groups and the community and voluntary sector.
The forum has recently recruited a patient representative with the support of Healthwatch.
Recommendation completed.
- NHS England, the ICB and the Community Pharmacy and Public Health Forum to ensure commissioned and delivered services are operating in line with NHSE's ‘Core20plus5’ approach to address health inequalities.
The overall aim is to improve health and well-being outcomes and reduce health inequalities for people in Brighton & Hove. This includes patients, service users, carers and local residents.
Health inequality workstreams are a standing item on the agenda, and the forum collaborates with other providers through the Brighton & Hove health inequalities collaboration and PCN Health Inequalities meetings. The Forum has also supported community events at the Hangleton and Knoll Project.
Community pharmacy locally commissioned services are reviewed in line with the needs in the city, and commissioning is adapted to reflect the needs of more vulnerable groups, with input from all parts of the system.
Recommendation completed.
Becoming carbon neutral
- NHSE, the Sussex ICB and BHCC commissioners to consider how to encourage, incentivise or commission community pharmacies to undertake further action on becoming carbon neutral. Plans to be monitored by the Community Pharmacy and Public Health Forum.
- The Community Pharmacy and Public Health Forum to work with the council’s Sustainability Team to support community pharmacies and those using them to contribute further to carbon reduction.
NHS Sussex has encouraged the use of lower-carbon inhalers, producing guidance on lower-carbon inhalers for clinicians and patients. Community pharmacies have been involved in this scheme by supporting patients who have changed to the lower-carbon inhaler devices.
A number of pharmacies across the city also offer recycling facilities for medicine blister packaging.
The Community Pharmacy and Public Health Forum intend to review sustainability initiatives and how they can support or incentivise further sustainable measures in Brighton & Hove.
Recommendations 23 and 24 not completed: Further work to be completed in this area.
Section 9: Future opportunities for possible community pharmacy services in Brighton & Hove
9.1 Introduction
Any local commissioning of services for delivery by community pharmacy lies outside the requirements of a PNA; it's considered as being additional to any Necessary Services required under the PLPS Regulations.
In reviewing the provision of Necessary Services and considering Advanced, National Enhanced and Locally Commissioned Services for Brighton & Hove as part of the PNA process, it was possible to identify opportunities for service delivery via the community pharmacy infrastructure that could positively affect the population.
Not every service can be provided from every pharmacy, and service development and delivery must be planned carefully. However, many of the health priorities, national or local, can be positively affected by services provided by community pharmacies, albeit being out of the scope of the PNA process.
9.2 Opportunities for pharmaceutical service provision
Health needs and the highest risk factors for causing death and disease for the Brighton & Hove population are stated in Sections 2 and 6. Should these be priority target areas for commissioners, they may want to consider the current and future service provision from community pharmacies, in particular, the screening services they are able to offer.
Based on these priorities and health needs, community pharmacy can be commissioned to provide services that can help and support the reduction of the variances seen in health outcomes across Brighton & Hove.
The PNA recognises the evolving role of community pharmacy in delivering preventive care, reducing health inequalities and integrating with PCNs.
While no gaps have been identified in the current or future (3-year) provision of pharmaceutical services in Brighton & Hove, there are opportunities to strengthen pharmacy services in alignment with the proposed NHS 10-Year Health Plan and Change NHS initiative. These opportunities focus on:
- prevention
- long-term conditions
- primary care access
- medicines management
- health inequalities
- integrated care
The most appropriate commissioning route would be through the ICS as Enhanced Pharmaceutical Services or through the local authority and locally commissioned services, which would not be defined as necessary services for this PNA.
Community Pharmacy England (CPE) commissioned leading health think tanks, Nuffield Trust and The King’s Fund, to develop a vision for community pharmacy to see a transformation of this sector over the next decade. These themes are reflected below.
Strengthening the role of community pharmacy in prevention, preventing ill health and supporting wellbeing
Community pharmacies should be fully integrated into preventive healthcare, supporting early detection, health promotion, and self-care initiatives.
Services such as the Hypertension Case-finding Service, Smoking Cessation Advanced Service, and NHS Health Checks should be prioritised to reduce the incidence of long-term conditions.
Reducing health inequalities through targeted pharmacy services
Commissioners should focus on increasing the uptake of Essential, Advanced, and LCS in areas of deprivation, ensuring equitable access to services such as sexual health, smoking cessation, cardiovascular risk screening and weight management.
Public awareness campaigns should be enhanced to improve access to pharmacy services, particularly for non-English-speaking communities and those facing healthcare access barriers.
Incentives should be considered for pharmacies in underserved areas to expand their service offering and address local health disparities, particularly where there is underprovision of LCSs.
Embedding pharmacy into integrated NHS neighbourhood health services, providing clinical care for patients
Community pharmacy should be positioned as a core provider within primary care, ensuring seamless referrals and collaboration between ICSs, local authorities and PCNs.
Medicines optimisation services, including repeat dispensing, the New Medicine Service, and the Discharge Medicines Service, should be embedded within primary care pathways to enhance patient safety and medication adherence.
Interdependencies between ICB and LCS services, such as smoking cessation and sexual health services, should be leveraged to provide more holistic and accessible care. This will require close ICB, local authority and Local Pharmaceutical Committee (LPC) collaboration.
Supporting workforce development and expanding pharmacy services
Sustainable funding should be prioritised to ensure the long-term stability and growth of community pharmacy services.
The ICB should explore commissioning a pharmacy workforce development programme, ensuring pharmacists and their teams are equipped to deliver expanded clinical services under the Community Pharmacy Contractual Framework (CPCF).
The introduction of independent prescribing for pharmacists from 2026 presents a significant opportunity for community pharmacies to manage long-term conditions and improve primary care access.
The pharmacy team’s role should be expanded, with pharmacy technicians supporting service delivery under Patient Group Directions (PGDs) and pharmacy staff providing Making Every Contact Count interventions.
Enhancing public awareness and digital transformation
Public education campaigns should be developed to raise awareness of pharmacy services, using diverse communication methods tailored to local communities.
Digital innovation should be prioritised, ensuring pharmacies have access to modern clinical decision-support tools and NHS-integrated patient records.
The adoption of point-of-care testing services in community pharmacies should be explored to improve early diagnosis and management of conditions such as diabetes, hypertension, and respiratory diseases.
Monitoring future demand and improving public engagement
The provision of pharmaceutical services should be regularly monitored and reviewed, particularly in light of demographic changes and population health needs.
Future PNAs should incorporate enhanced stakeholder and public engagement strategies to ensure services reflect local priorities and community health needs.
Community-based medicines management: Living well with medicines
Community pharmacy provides patient access to a local expert to support advice and safe access to medicines.
The growth of independent prescribing in community pharmacy offers greater opportunities to take pressure off general practice and shared responsibilities, managing prescribing budgets and delivering structured medication reviews.
These services could be offered as part of domiciliary services to housebound patients and care homes.
By aligning with national health priorities, these considerations/recommendations ensure that community pharmacy plays a central role in being part of an integrated neighbourhood in:
- delivering preventive care
- tackling health inequalities
- supporting long-term condition management
This will ultimately improve the health and well-being of Brighton & Hove residents.
9.3 Future opportunities specific to Brighton & Hove
Local authority and Sussex ICB to formally embed community pharmacies within prevention strategies at the neighbourhood and PCN level, ensuring pharmacies are recognised as first-line providers for public health interventions, screening, and early detection activities.
As commissioning for vaccination services transitions to the ICB in 2026, there is an opportunity to expand pharmacy delivery beyond flu and COVID-19 to include pneumococcal, shingles, and RSV vaccinations, supporting early prevention and population immunisation targets. This builds on the recommendation from the previous PNA.
A targeted public awareness campaign should be developed to raise awareness of preventive health services available through community pharmacies, ensuring communication reaches underserved populations and those with the highest health risks, aligning with the ‘PLUS5’ groups for Brighton & Hove.
Sussex ICB and Public Health should consider developing incentives for pharmacies located in under-served or deprived areas to expand delivery of Locally Commissioned Services, particularly services like sexual health advice.
Sussex ICB, PCNs, and Brighton & Hove City Council should look to formally integrate community pharmacy services into neighbourhood multidisciplinary teams, enabling seamless referral pathways between general practice, pharmacy, and other primary care services.
Sussex ICB should work with Community Pharmacy Surrey and Sussex (LPC) to commission a pharmacy workforce development programme, focusing on clinical skills development and service delivery under the Community Pharmacy Contractual Framework (CPCF), and preparation for independent prescribing.
System partners should prepare to maximise the opportunity presented by independent prescribing from 2026 by:
- identifying early pharmacy prescribers
- supporting mentoring and supervision arrangements
- aligning service pathways to support pharmacies managing common conditions and long-term diseases
Building a digitally connected, accessible, and well-informed community pharmacy network will be vital to improving early diagnosis, empowering residents to manage their health, and supporting integrated and person-centred care across Brighton & Hove.